With amyloidosis being such a rare but brutal disease, the fact that it is so misunderstood and diagnosis is often delayed beyond treatment means that promoting awareness is critical. Chris and I remain incredibly lucky that she read the news article about Jenifer Gershman in the newspaper. http://www.metrowestdailynews.com/archive/x1853598606 It pointed Chris to the diagnosis and allowed us a strong treatment. Everyone we speak to who suffers from this disease is amazed that Chris went from her first significant symptoms in January to diagnosis in April, to stem cell transplant/chemo in June. We were very aggressive about testing and treatment, but very lucky as well. Jenifer made a commitment to promote awareness with the hope that she could help others with an early diagnosis, and with Chris she succeeded. Now it is time to help Jenifer, and that is one of the reasons Stephen has decided to do the 1500 mile bike ride. This will be an incredible accomplishment, but I am sure he will pull it off, even if he rides in snow storms in the night. But even more incredible is the response he has received from so many people. It has blown him and us away at the generosity and willingness to help to raise this money for the Amyloidosis Research Foundation. He will be updating the status of things as this is completely his initiative, but suffice it to say the outpouring has been fantastic so far. He has tremendous support from sponsors from diverse as bike retailers to cookie companies to landscape architects. The sponsors then help him raise the money by supporting the cost of the ride itself. Stephen will of course give 100% of the donations to the foundation. Those donations are coming in daily in the mail or on the foundation web site. I cannot tell you how very much appreciated these are. Some are small and some are big, but Stephen just can't believe the number of donors. Even his friends at school have been raising money through various events. Just amazing. Stephen is as much interested in the number of donors as the amount, as it means that someone was willing to spend the few minutes it took to help promote awareness of Chris' disease. Thus, even small donations are very appreciated as it means one more person helps fight the cause.
Stephen has had some good press on his campaign. The regional newspaper came by and interviewed Chris and Stephen for their Sunday edition. Here is the link:
http://www.metrowestdailynews.com/archive/x1556828605/Spitz-Son-is-riding-for-moms-life
Chris continues to work hard at regaining her strength and fitness. Unfortunately the bad weather does not encourage much outdoor exercise. Her aerobic fitness is very important to her heart, so she tries when she can, but still feels very winded with her reduced heart function. Her cocktail of pills continues morning and night, but she has not complained about it. I am becoming more convinced based on conversations with doctors and my own knowledge of the disease that Chris will be doing oral chemo this spring or summer. We need to attack the remaining proteins (lamda light chains) still being produced and prevent any further deposition in her organs, especially her heart. The March visit will be the point where we decide the next steps. Chris keeps saying, "I just want to know where I stand", as we feel like we have more to do but no definitive action plan. But in about 4 weeks we will know, just as Stephen starts his ride.
Again here is the link to his site: http://chrisjourney.com/
Thanks to all.
Tuesday, February 3, 2009
Friday, January 30, 2009
A very brief photo history: To Hell and Back
 Chris and her sister Debbie in August of 2007 in NH. We had no idea what the next 12 months would bring at this point.
Chris and her sister Debbie in August of 2007 in NH. We had no idea what the next 12 months would bring at this point.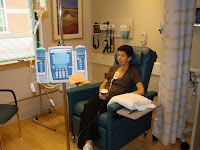 June 2008 - Getting ready to start the chemo. It took about 15 minutes to take it all. Notice the "pic" line inserted in her chest. The chemo was given via the line. The chemo is so strong that it can burn through veins close to the skin, thus Chris had to keep ice packed in her mouth for about 20 minutes to avoid severe sores. This is the equivalent of 6 months worth of oral chemo in two direct shots over 2 days.
June 2008 - Getting ready to start the chemo. It took about 15 minutes to take it all. Notice the "pic" line inserted in her chest. The chemo was given via the line. The chemo is so strong that it can burn through veins close to the skin, thus Chris had to keep ice packed in her mouth for about 20 minutes to avoid severe sores. This is the equivalent of 6 months worth of oral chemo in two direct shots over 2 days.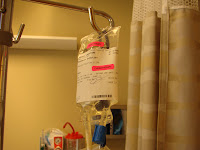 The actual chemo, melphalan, which was given via the pic line (catheter) that had been inserted into her chest for about 6 weeks. This is the stuff that almost kills you but in the end is your best friend. Chris took the maximum (but highest risk) dose.
The actual chemo, melphalan, which was given via the pic line (catheter) that had been inserted into her chest for about 6 weeks. This is the stuff that almost kills you but in the end is your best friend. Chris took the maximum (but highest risk) dose.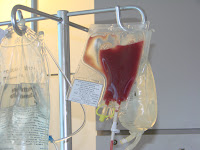 One of two bags, each containing 5 million stem cells. These are collected in a process similar to dialysis and separated with a centrifuge. The stems cells are collected prior to the chemo, then replanted a few days afterward.
One of two bags, each containing 5 million stem cells. These are collected in a process similar to dialysis and separated with a centrifuge. The stems cells are collected prior to the chemo, then replanted a few days afterward.Tuesday, January 27, 2009
Another Echo today
Chris had another Echocardiagram today with Dr Falk to get his most recent perspective on her heart status. He compared the results with the November echo and saw no change, either good or bad. He is waiting to get the May echo from BU and then will compare that to the one today to see what has really occurred over the last 8 months or so. This will give us the widest possible spread of dates and provide an indication of how things have changed. The May echo was her first. So really not any significant news other then we remain concerned about the overall status of her heart and its ability to keep up with an active lifestyle.
Chris did go to Yoga again and she really feels like this is good for her. She complains that she feels very tight and yet she is pleased with her strength. Hopefully she will keep this up, as well as more cardio exercise. The weather has been very bad here and this limits the outside walks of course.
Last week I was in Rochester, MN for a business meeting and I made a trip to the Mayo Clinic which is really the only other amyloidosis center in the world, or at least the US. Rochester is a very funny place as it is about 90 miles from Minn./St Paul and really has two major employers: Mayo and IBM. The Mayo clinic of course is world renowned for it's expertise and incredible staff, but you have to wonder how it ended up in Rochester. The facility itself is amazing. I am not kidding when I say that the lobby is a beautiful three story atrium and there is a man in a tux playing a grand piano. I felt as if I was in the Four Seasons hotel. It must be hard for those without health insurance or needing to cover ongoing medical bills to see this use of money, but it certainly was an incredible place. What I really wanted to see was the Amyloidosis Center, just to see what it looked like compared to BU. We had heard of many patients who had been to Mayo for clinics or evaluation and thus it would be interesting to see it. I asked at the front desk and of course they had never heard of amyloidosis and had no idea where to direct me. Then I asked where the Hematology dept was and they said the 10th floor which I then proceeded to go investigate.
I was looking for a picture of the Center, just a nameplate or a logo or something that indicated Mayo and Amyloidosis as I wanted to give it to Stephen for his fund raiser web site (http://chrisjourney.com/) A woman that worked in the Hematology dept asked if she could help (as I wandered around aimlessly) and I explained what I was looking for. She went back to the inner sanctum of the hospital and returned saying that she had asked one of the doctors, Dr. Morie Gertz, if he knew of a sign or poster or something that I could take a picture of and the answer was simply "nope, nothing like that". Oh well. Interestingly as she mentioned Dr. Gertz' name, it hit me that I had read many many publications of his in my quest to be the expert on this disease. I brazenly asked if I could quickly meet him, just to say hello and tell him how appreciative I was of his work (and maybe get a quote for Stephen's bike ride). She went back to ask and returned with a curt "he is unavailable". My intentions were very honorable, but oh well, it just did not work out.
So our next major step is to hear about the comparison of May's echo with the one today with Dr Falk. Ideally we will get some important insight into the real level of her ejection fraction. This is a big frustration to Chris and I as we really do not have consistent answers. Hopefully we will learn more in the next few days.
Chris has recently heard from a number of friends who had not heard of her illness. She is really glad to hear from them and as always I encourage everyone to please feel free to call her. The support from all just continues to energize her. Thanks to all who have reached out in so many ways.
Chris did go to Yoga again and she really feels like this is good for her. She complains that she feels very tight and yet she is pleased with her strength. Hopefully she will keep this up, as well as more cardio exercise. The weather has been very bad here and this limits the outside walks of course.
Last week I was in Rochester, MN for a business meeting and I made a trip to the Mayo Clinic which is really the only other amyloidosis center in the world, or at least the US. Rochester is a very funny place as it is about 90 miles from Minn./St Paul and really has two major employers: Mayo and IBM. The Mayo clinic of course is world renowned for it's expertise and incredible staff, but you have to wonder how it ended up in Rochester. The facility itself is amazing. I am not kidding when I say that the lobby is a beautiful three story atrium and there is a man in a tux playing a grand piano. I felt as if I was in the Four Seasons hotel. It must be hard for those without health insurance or needing to cover ongoing medical bills to see this use of money, but it certainly was an incredible place. What I really wanted to see was the Amyloidosis Center, just to see what it looked like compared to BU. We had heard of many patients who had been to Mayo for clinics or evaluation and thus it would be interesting to see it. I asked at the front desk and of course they had never heard of amyloidosis and had no idea where to direct me. Then I asked where the Hematology dept was and they said the 10th floor which I then proceeded to go investigate.
I was looking for a picture of the Center, just a nameplate or a logo or something that indicated Mayo and Amyloidosis as I wanted to give it to Stephen for his fund raiser web site (http://chrisjourney.com/) A woman that worked in the Hematology dept asked if she could help (as I wandered around aimlessly) and I explained what I was looking for. She went back to the inner sanctum of the hospital and returned saying that she had asked one of the doctors, Dr. Morie Gertz, if he knew of a sign or poster or something that I could take a picture of and the answer was simply "nope, nothing like that". Oh well. Interestingly as she mentioned Dr. Gertz' name, it hit me that I had read many many publications of his in my quest to be the expert on this disease. I brazenly asked if I could quickly meet him, just to say hello and tell him how appreciative I was of his work (and maybe get a quote for Stephen's bike ride). She went back to ask and returned with a curt "he is unavailable". My intentions were very honorable, but oh well, it just did not work out.
So our next major step is to hear about the comparison of May's echo with the one today with Dr Falk. Ideally we will get some important insight into the real level of her ejection fraction. This is a big frustration to Chris and I as we really do not have consistent answers. Hopefully we will learn more in the next few days.
Chris has recently heard from a number of friends who had not heard of her illness. She is really glad to hear from them and as always I encourage everyone to please feel free to call her. The support from all just continues to energize her. Thanks to all who have reached out in so many ways.
Friday, January 23, 2009
Brief Update on the Cardiologist meeting
Well, it is hard to say that Chris and I walked away with some incredible earth shaking news from the appointment with Dr Falk yesterday. We spent almost an hour with him reviewing his analysis, what the results show, next steps, etc. At the end, I asked him to summarize all of our discussions in just a few words. and he said, as he counted the words on his fingers: "I think she is doing very well".
Chris and I don't know exactly how to react to that. He did indicate that there has in fact been some decline in the heart function, as measured by the ejection fraction. He does not believe it is nearly as bad as the most recent BU analysis says, but he thinks there is some detioration since May. He did not know if that was due to further amyloid deposition in her left ventricle, or possibly the result of the high dose chemo itself. What confuses him (or as he says is "a contraindication") is that all of her other organs have responded so well to the treatment. Like Dr. Sanchorawala at BU, he says she clearly has had a very good partial response, but not the complete response we were all praying for. As such we asked him the likely next steps and he laid out pretty much the same 4 options we knew. 1) Another stem cell with high dose chemo, 2) oral Velcade, 3) oral Revlimid and 4) do nothing. Of course option 4 is not an option for me, so we ignore that. He doubts that any incremental benefits of the stem cell/chemo approach would be worth the risk due to her heart condition (the benefit being negligible vs a higher risk for cardiac involved patients). He thought the the oral Velcade would be his choice but he was clear to point out that he trusts BU and in the end that is a call they (and us) need to make.
He does want another (yes, yet another) echo next week. That way, they will have one more data point. One from BU in May, Dr Falk in November, BU again in December, and Dr Falk again in January. As echo's cause no radiation, I think getting more history for analysis is the right thing to do.
We did discuss mitral valve leakage and he stated that while there is probably some there, it was not a huge issue and there would be no action to take even if it was, as surgery would not be viable.
Chris asked the burning question "Can I ski ?". He was not very positive on that as he was afraid that any potential low blood pressure might cause her to faint and hit a tree. It was not a concern about stress on the heart from skiing, but a concern about fainting. Nevertheless, Chris and I did agree that on a beautiful sunny, non crowded day in March, we will in fact go ahead and ski. Chris enjoys skiing, is very good at it, and the hell with it, if we take it easy we can have a great day. So look for us in March on the slopes. I am not denying her of this and we set it as a goal.
Chris will get the results of next weeks echo right away, so we will have new news next week. I also need to add pictures here as I promised (but Stephen has beaten me to the punch on his 1500 mile ride for amyloidosis web site). Thanks for checking in and caring so much about Chris. As the doctor said, "She is doing great", but it just does not seem like we are yet able to close the book on this journey to good health. We are getting there however, I am very optimistic.
Please feel free to call Chris, she would love to hear from you and it is important for her to talk.
Pictures soon.
A small minor point: I am writing this post from Rochester MN, home of the other Amyloidosis Center. If I get a chance I may stop in to see the center.
Chris and I don't know exactly how to react to that. He did indicate that there has in fact been some decline in the heart function, as measured by the ejection fraction. He does not believe it is nearly as bad as the most recent BU analysis says, but he thinks there is some detioration since May. He did not know if that was due to further amyloid deposition in her left ventricle, or possibly the result of the high dose chemo itself. What confuses him (or as he says is "a contraindication") is that all of her other organs have responded so well to the treatment. Like Dr. Sanchorawala at BU, he says she clearly has had a very good partial response, but not the complete response we were all praying for. As such we asked him the likely next steps and he laid out pretty much the same 4 options we knew. 1) Another stem cell with high dose chemo, 2) oral Velcade, 3) oral Revlimid and 4) do nothing. Of course option 4 is not an option for me, so we ignore that. He doubts that any incremental benefits of the stem cell/chemo approach would be worth the risk due to her heart condition (the benefit being negligible vs a higher risk for cardiac involved patients). He thought the the oral Velcade would be his choice but he was clear to point out that he trusts BU and in the end that is a call they (and us) need to make.
He does want another (yes, yet another) echo next week. That way, they will have one more data point. One from BU in May, Dr Falk in November, BU again in December, and Dr Falk again in January. As echo's cause no radiation, I think getting more history for analysis is the right thing to do.
We did discuss mitral valve leakage and he stated that while there is probably some there, it was not a huge issue and there would be no action to take even if it was, as surgery would not be viable.
Chris asked the burning question "Can I ski ?". He was not very positive on that as he was afraid that any potential low blood pressure might cause her to faint and hit a tree. It was not a concern about stress on the heart from skiing, but a concern about fainting. Nevertheless, Chris and I did agree that on a beautiful sunny, non crowded day in March, we will in fact go ahead and ski. Chris enjoys skiing, is very good at it, and the hell with it, if we take it easy we can have a great day. So look for us in March on the slopes. I am not denying her of this and we set it as a goal.
Chris will get the results of next weeks echo right away, so we will have new news next week. I also need to add pictures here as I promised (but Stephen has beaten me to the punch on his 1500 mile ride for amyloidosis web site). Thanks for checking in and caring so much about Chris. As the doctor said, "She is doing great", but it just does not seem like we are yet able to close the book on this journey to good health. We are getting there however, I am very optimistic.
Please feel free to call Chris, she would love to hear from you and it is important for her to talk.
Pictures soon.
A small minor point: I am writing this post from Rochester MN, home of the other Amyloidosis Center. If I get a chance I may stop in to see the center.
Monday, January 19, 2009
1500 Miles (click here)
All of our children have been the best possible supporters of Chris throughout her journey to health. They have sacrificed a great deal to ensure that they can help Chris however she needs it; around the house, giving up activities, running errands, and keeping things going at home while Chris went through her Chemo in Boston.
Fortunately, our 17 year old son Stephen has a unique opportunity to help in another way. During a 2 week spring-break in March, he and some of his close friends have organized a fund-raiser with all of the proceeds going to the Amyloidosis Research Foundation. He and others (sponsors, friends) will bear all of the expenses ensuring that every dollar that is donated will go directly to the foundation. His ride will take him from Florida to Massachusetts over a 2 week period. This will mean he will need to cycle an average of over 115 miles everyday for 14 days - an incredible challenge. His goal is to raise $10,000 during this ride while promoting awareness.
A link to the web site he has created is on the right side of the blog. He is anxious to get a strong start toward his goal, and has already lined up sponsors who will support the ride. Any donation of any value will be greatly appreciated. This is fully tax deductible and will represent a very important donation towards the fight against Amyloidosis. Chris has been extremely fortunate that we have the medical care, the financial resources, a supportive community, and amazing friends who have all been an important part of Chris' journey. What Stephen wants do to is to help others who may not be so fortunate in their fight. Chris continues to fight, and we are sure she will win, but their are many others who can be helped by awareness, research, treatment, and support. This is his objective - not bad for a 17 year old kid.
Feel free to contact him with questions at: stephen@chrisjourney.com and please follow his blog as he prepares and then completes the ride. Chris and I thank you very much.
Fortunately, our 17 year old son Stephen has a unique opportunity to help in another way. During a 2 week spring-break in March, he and some of his close friends have organized a fund-raiser with all of the proceeds going to the Amyloidosis Research Foundation. He and others (sponsors, friends) will bear all of the expenses ensuring that every dollar that is donated will go directly to the foundation. His ride will take him from Florida to Massachusetts over a 2 week period. This will mean he will need to cycle an average of over 115 miles everyday for 14 days - an incredible challenge. His goal is to raise $10,000 during this ride while promoting awareness.
A link to the web site he has created is on the right side of the blog. He is anxious to get a strong start toward his goal, and has already lined up sponsors who will support the ride. Any donation of any value will be greatly appreciated. This is fully tax deductible and will represent a very important donation towards the fight against Amyloidosis. Chris has been extremely fortunate that we have the medical care, the financial resources, a supportive community, and amazing friends who have all been an important part of Chris' journey. What Stephen wants do to is to help others who may not be so fortunate in their fight. Chris continues to fight, and we are sure she will win, but their are many others who can be helped by awareness, research, treatment, and support. This is his objective - not bad for a 17 year old kid.
Feel free to contact him with questions at: stephen@chrisjourney.com and please follow his blog as he prepares and then completes the ride. Chris and I thank you very much.
Saturday, January 17, 2009
Doing Well - Waiting for 1/22 Cardiac Appt
Chris has had a good couple of weeks. She has been busy with various trips to Vermont and NY, putting away all the Christmas things, getting back to yoga, etc. She really was glad to start the yoga again and she said she felt stronger than she expected. This was encouraging and I expect she will continue this and soon get back to the gym where she was a regular less than a year ago. The yoga is also important for her mental health (or so she tells me), but I hope I don't come home some day and find a Yogi humming in our living room.
We received the full report from our BU visit back in mid-December. The entire report is 40+ pages as all of the results are included from the lung, heart, kidney, blood and liver tests. I will map the data against the trend charts as a measure of ongoing improvement. I thought I would include some comments from the summary here as an example of the results. These are all quotes:
-On physical examination, Mrs Wright looked well. She was aferbrile with a standing heart rate of 104 bpm and a corresponding blood pressure of 92/61 (mmHg). She was not orthostatic. HEENT exam revlealed no submandibular gland enlargement.
-Cardiac auscultation revelaed a regular rate and rythm without murmer.
-Pulmonary auscultation revelaed mild bibasilar crackles.
-Mrs. Wright underwant numerous diagnostic tests during the course of her eevaluation with us. Serum immunofixation revealed a polyclonal distribtion with a persistent, but fainter IgM lambda band. A pevious M-spike of 0.42 has now essentially resolved.
-Transthoracis echocardiogram notes worsening of left ventricular ejection fraction at 35% with the suggestion of worsened mitral regurgitation and persistent biatrial enlargement. Dr. (I will leave the name out here) noted her echo findings seemed contradictory to her improved functional status with decreasing need for medication.
-Dr. Sanchorawala noted that Mrs. Wright has had a great partial response of her underlying plasma cell dyscrasia and evidence of protein response with a reduction in proteinuria, BNP, diuretic requirement, and improves tolerance. Dr. Sanchorawala advises no additional treatment is needed at this time; however, she did request that Mrs. Wright return to clinic in 3 months (March 8-10) for reevaluation to include serum free light chain analysis.
Imagine 40 pages of this. So what does this all mean? Here is where I think we are as of Jan. 17.
Chris clearly has had a very good response to the chemo therapy. The amyloid proteins in both her blood and her urine are down significantly, yet she has not had the Complete hematological response we were all hoping for. Yet, she is 95% there. She is really feeling very good and her stamina, attitude, and outlook are all positive. She is getting herself into a normal routine and really feeling good about things. The worry however is clearly the heart. She is formally in congestive heart failure (you would never know it) and we have the entire spectrum of numbers around the ejection fraction - ranging from 50% to 20% ( normal is 55%-75%). As such, our next major gate is meeting with Dr. Falk, the amyloidosis cardiologist specialist on Jan 22. We have sent him the actual CD of the echo from BU and he will review that vs his own offices tests and the one done at Brigham and Women's and see what the heck is the real truth.
Chris has restarted the Coumadin (blood thinner) and has had no adverse reaction, unlike the first attempt. I now blame that reaction to Thai food (so thankfully we won't be going back to that restaurant soon). We'll see what Dr. Falk says about the implications for using this for the rest of her life, but I anticipate that is going to be the reality as it is needed to prevent a stroke from a thrombosis in her heart.
Stephen has been working very diligently on his required senior high school project which is to raise funds and awareness for Amyloidosis. He has 2 weeks off from school in March and his plan is to ride from Florida to Massachusetts. He is developing a web site, mapping the ride, creating a budget, etc. He has contacted the Amyloidosis Research Foundation as well as local sponsors - all on his own. Chris and I are very impressed with his passion and determination. He has asked for no help at all from us as he really wants to do this on his own. I am asking if I can at least join his support crew - he'll "think about it". His plan is to do this in the first 2 weeks of March, so time is now critical to get the plan locked, but I am sure he will make this happen. I will be posting a link to his web site in the next week or so.
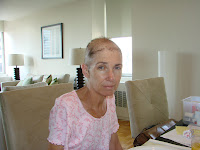
I also have permission from Chris to post some pictures of her over the last few months. Many of her distantly located friends have been asking for pictures and she has always said no, but now she feels as if it might make people more aware if she can show them how you can come back from the hell of the high dose chemo. So I will look for some and post them here in the next week. She will of course maintain editorial control she warns me.
Again my apologies for my delayed blog updates. I have started a new ( and very exciting) job at IBM and am in the middle of reshuffling organizations. Yet job #1 remains Chris. I will certainly post an update after the cardiac appointment and hopefully post some pictures in the next few days.
A million thanks for your ongoing interest and support. I can't tell you how important it is.
We received the full report from our BU visit back in mid-December. The entire report is 40+ pages as all of the results are included from the lung, heart, kidney, blood and liver tests. I will map the data against the trend charts as a measure of ongoing improvement. I thought I would include some comments from the summary here as an example of the results. These are all quotes:
-On physical examination, Mrs Wright looked well. She was aferbrile with a standing heart rate of 104 bpm and a corresponding blood pressure of 92/61 (mmHg). She was not orthostatic. HEENT exam revlealed no submandibular gland enlargement.
-Cardiac auscultation revelaed a regular rate and rythm without murmer.
-Pulmonary auscultation revelaed mild bibasilar crackles.
-Mrs. Wright underwant numerous diagnostic tests during the course of her eevaluation with us. Serum immunofixation revealed a polyclonal distribtion with a persistent, but fainter IgM lambda band. A pevious M-spike of 0.42 has now essentially resolved.
-Transthoracis echocardiogram notes worsening of left ventricular ejection fraction at 35% with the suggestion of worsened mitral regurgitation and persistent biatrial enlargement. Dr. (I will leave the name out here) noted her echo findings seemed contradictory to her improved functional status with decreasing need for medication.
-Dr. Sanchorawala noted that Mrs. Wright has had a great partial response of her underlying plasma cell dyscrasia and evidence of protein response with a reduction in proteinuria, BNP, diuretic requirement, and improves tolerance. Dr. Sanchorawala advises no additional treatment is needed at this time; however, she did request that Mrs. Wright return to clinic in 3 months (March 8-10) for reevaluation to include serum free light chain analysis.
Imagine 40 pages of this. So what does this all mean? Here is where I think we are as of Jan. 17.
Chris clearly has had a very good response to the chemo therapy. The amyloid proteins in both her blood and her urine are down significantly, yet she has not had the Complete hematological response we were all hoping for. Yet, she is 95% there. She is really feeling very good and her stamina, attitude, and outlook are all positive. She is getting herself into a normal routine and really feeling good about things. The worry however is clearly the heart. She is formally in congestive heart failure (you would never know it) and we have the entire spectrum of numbers around the ejection fraction - ranging from 50% to 20% ( normal is 55%-75%). As such, our next major gate is meeting with Dr. Falk, the amyloidosis cardiologist specialist on Jan 22. We have sent him the actual CD of the echo from BU and he will review that vs his own offices tests and the one done at Brigham and Women's and see what the heck is the real truth.
Chris has restarted the Coumadin (blood thinner) and has had no adverse reaction, unlike the first attempt. I now blame that reaction to Thai food (so thankfully we won't be going back to that restaurant soon). We'll see what Dr. Falk says about the implications for using this for the rest of her life, but I anticipate that is going to be the reality as it is needed to prevent a stroke from a thrombosis in her heart.
Stephen has been working very diligently on his required senior high school project which is to raise funds and awareness for Amyloidosis. He has 2 weeks off from school in March and his plan is to ride from Florida to Massachusetts. He is developing a web site, mapping the ride, creating a budget, etc. He has contacted the Amyloidosis Research Foundation as well as local sponsors - all on his own. Chris and I are very impressed with his passion and determination. He has asked for no help at all from us as he really wants to do this on his own. I am asking if I can at least join his support crew - he'll "think about it". His plan is to do this in the first 2 weeks of March, so time is now critical to get the plan locked, but I am sure he will make this happen. I will be posting a link to his web site in the next week or so.
I also have permission from Chris to post some pictures of her over the last few months. Many of her distantly located friends have been asking for pictures and she has always said no, but now she feels as if it might make people more aware if she can show them how you can come back from the hell of the high dose chemo. So I will look for some and post them here in the next week. She will of course maintain editorial control she warns me.
Again my apologies for my delayed blog updates. I have started a new ( and very exciting) job at IBM and am in the middle of reshuffling organizations. Yet job #1 remains Chris. I will certainly post an update after the cardiac appointment and hopefully post some pictures in the next few days.
A million thanks for your ongoing interest and support. I can't tell you how important it is.
Sunday, January 4, 2009
Lessons Learned from Chris' Journey through 2008
With 2008 gone, and our optimism for a much better 2009 as high as ever, I have thought for awhile now that it would be important to share my insights, perspectives, recommendations, and warnings for others who may be face a similar circumstance, I will try not to be too verbose (yeah right) but convey the essence of the thought. Some of these may be only applicable to Amyloidosis, but I am trying to think of them more generally. So here goes:
-If your family member, colleuege, neighbor, whomever says, "I'm just not feeling right" or "something is wrong but I can't tell you what" and this goes on for an extended period (more than a few weeks), get it checked out. Don't write it off to old age or work stress or a low-grade fever. I am convinced the body sends the mind clear messages that attention is needed. If something isn't feeling right, then do somehting about it. We all want to fight the battle, keep moving, go to work, etc. We don't have time for the Doctor. Lesson: If you don't feel well for more than a few weeks, see a doctor. Time may be very important. Many Amyloid patients miss their opportunity for treatment because they were not diagnosed early enough. They die from a lack of a diagnosis.
-Get a second opinion on anything more than the basics. As I have stated many times, medicine is an art not a science. What one doctor misses, the other may see. Every doctor has a different set of experiences and training. They use their judgement based on what they know. The experts based at the BU center believe that >95% of primary care physicians have never diagnosed nor treated Amyloidosis and would not even think of testing for it. Maybe they read about it in Medical School. This is why the majority of sufferers die from the disease before treatment. Doctors don't see it, they don't know what too look for, and they don't even think to test for it. A great book to read if your looking for something on this topic is a book I happened to have read about a year ago. It is very interesting reading for a caregiver or advocate:
http://www.amazon.com/How-Doctors-Think-Jerome-Groopman/dp/0618610030 (sorry I don't mean to promote Amazon). I strongly recommend it before a crisis hits and I am sure it shaped my own thinking as Chris' advocate.
Have an annual physical with complete blood and urine tests. The body is filled with bio-markers which are indicators of chemical balance. I had no idea how complicated the chemical make-up of the human body is until I looked at a 5 page blood analysis. We have every metric on Chris since May and each one tells a story: glucose, potassium, protein, lambda light chains, albumin, creatinine, etc, etc...... Always have complete blood work and a urinalysis at every checkup. and always have it if you are going in if you don't feel well. Be aggressive about getting these done, they are not needless tests, they are critical chemical indicators. Chris had a urine test, which then led to a 24 hour urine analysis, which then led to an indication of an immuniglobulin M-spike, which then led to a bone marrow biopsy, and then a fat-pad biopsy that was tested with the famous red congo stain confirming Primary Amyloidosis. Without the first urine test, the whole sequence would have been delayed and the diagnosis may never have happened.
Become an expert. Whether it is heart disease, lung cancer, pneumonia, or any strange disease nobody has ever heard of, the resources are there to become an expert. The more you know, the more you become a participant in the discussion with the medical team vs an observer to the process. You can challenge, ask intelligent questions, seek out specialists, manage the drugs, demand tests, and potentially avoid problems. I now know drug interactions, I know all clinical trials by drug companies, I know the latest testing techniques, and I have read almost every paper written in the last few years on the subject. I use Google Alerts to scan the Internet for all mention of Amyloidosis as well as any publications from selected experts in the field. I get a weekly update on all new items about the disease, including new trials, published studies, conferences, etc. I suggest reading all recently published works. In our case it comes form magazines such as Blood, Journal of the British Hematological Society, etc.
Document and get a copy of everything. I have a copy of every single test result Chris has had. I have a copy of every report written by every doctor. I have the daily blood tests results as well as the graphs of the trends over the entire period. These are documents that are your right to have as they are about you or the patient you are advocating for. I used to think there was some special underground/behind the scenes data that only the medical experts had access to. In fact you have rights to everything. There are many benefits to this:
-You can become smarter by looking up every term used, understanding every test result, and getting a very well documented position of the doctors opinion.
-You can make these available to other doctors who need to know the background, especially those providing a second opinion.
-You might be able to avoid tests. Chris has had many many lung x-rays. I am concerned about over use of these. With a copy of the x-rays, I simply hand them to another doctor and avoid the tests. As I have learned, hospitals operate as members of competitive organizations. They often network well inside of their partnership, but not well outside to other partnerships.
Hospitals are very infectious places. One surprising lesson I have learned is how hospitals are really filled with germs. Chris' immunity system was completely wiped out, and they did not want to have her stay in the hospital for fear of infection. Some hospitals do the stem cell transplant and high-dose chemo as in-patient. Boston Medical insists that all patients live off-site, but close. The doctors strongly believe that they have a lower mortality rate simply due to the number one cause of death for these patients - infections. I am not advocating that patients avoid the hospital, but I was surprised at how many stories I heard about people getting very serious infections in the hospital such as MRSA, staff infections, etc.
There are two critical roles: Caregiver and Advocate. These can be the same person or two different people, but they both need to be in place. The caregiver is focused on the patient and his/her comfort. All seriously ill patients need a caregiver, even if at the hospital. Nurses have many patients to worry about cannot give the level of comfort or attention that an ill patient really needs. The caregiver needs to do a virtual brain transplant and think in the mind of the patient. What would make them more comfortable, who might they be worrying about, what are they feeling? The caregiver needs to swallow their pride completely. As Steve G, husband of Jen (the couple whom we read about in the paper back in May) told me," be prepared to wear a loincloth, you will become a slave and will need to swallow all pride and be a servant". This is a tough and frustrating job. You may be asked to get something very small from a sound sleep, you may have to clean up some really nasty stuff, you may be sent to the store to get something only to find it was the wrong thing. My suggestion is to just acknowledge that you are there to serve. It is not about you, it is totally, 100% about the patient. You get very little sympathy, very little acknowledgement, and few people understand what you are personally going through. Suck it up, be tough, and focus only on the patient. You will have to run on the internal pride you will develop that you are making a difference.
The other key role is the medical advocate. This is the person who needs to be the brains to the caregivers heart. Write everything down, understand all medications, understand the rationale behind all tests. If there is a need for medical attention, go get it. Get the best you can, even if you have to fight a battle. Question everything -not to dispute it, but to understand it. Bring a notebook to all medical appointments and listen in on all medical rounds if in the hospital. Listen very carefully and then question for clarity. Since medicine is an art, not a science, there is no simple algorithm that doctors use to come up with the answer. The advocate needs to be a part of the decision making process if the patient cannot be. Don't let things happen around you with others making the decision, be a part of the decision. Be aggressive, actively representing the patient. This does not mean being a pain in the ass. I have asked the doctors at BU if they thought I was overly aggressive and a negative in the process. The answer is always: "active participation is always better than benign neglect". Yes, I asked alot of questions and yes I knew what I was talking about (sometimes not as much as I thought I did), but they respected me for being involved. I witnessed some spouses who did not go into an appointment with the doctor, could not even properly say the disease, had no idea what was going on, and thus could not advocate. The advocate is not about making the patient comfortable (that is the caregiver), but it is about fighting the required battles in the complex medical system we live in. It is very hard to do both, but it can be done. Just think of them as two different roles and understand which one your in. The caregiver has no pride and a big heart, the advocate has a big brain and a strong enough ego to go into battle if required. (As I right this, I know it sounds so obvious to most of us, but I witnessed such distant participation and bad care giving by family members that it shocked me).
Hospital chairs are terrible beds. It is a very small price to pay from what Chris has been through, and as the caregiver in the hospital, Chris wanted me there at night. But, these chairs are torture devices. The interesting thing is the difference in the patients. I had a very big back operation a year ago and was in the hospital for a week. The absolute last thing I would want is for Chris to be there overnight. In fact her being there for more than an hour was tough. When I am sick, just leave me alone, don't ask me how I am doing, just let me be and I will let you know when I am better and I'll call you to come pick me up. Chris is the opposite. She wanted me there every night and all day. I had to just accept it (the caregiver has no rights to personal comfort as the lowest form of life on earth) and sleep in a chair. Forget the previously cured back, but that is another story. The nurses were always very good about finding me a blanket and pillows and sneaking me a muffin or a soda, but all I can suggest is try to avoid these chairs as best you can. Again, a very small price to pay and probably my only complaint worth sharing.
Rely on religion, meditation, poems, psychologists, or denial - whatever works. The human mind is sometimes the patients worst enemy. Chris and I spent many many nights up all night, scared to death of our future, what would happen to our fantastic life, will we ever get through this, etc. Many tears, night sweats, all night pacing, it was horrendous. We both needed help, some kind of guidance. Chris reached out to many alternatives: our minister, prayer books, meditation, Reiki, massage, acupuncture, lucky bracelets from the kids, etc. Each worked a little and helped in the total picture. One thing that I found interesting was when we met with the Psychiatrist at BU as part of the normal regiment. He told us a very effective coping mechanism was the use of denial as a way to deal with this. Deny that anything could go wrong, deny that this is really happening, deny that there will be any changes in your life. He told us that this is how many patients cope. To me, it is a dangerous approach, but probably very effective. Chris found her prayer book very useful as she went to bed. It focused on hope, life, and love. She also got a bracelet from a good friend that said: Expect Miracles, Have Faith. She wears it daily and really believes that with faith, miracles can happen. One point I think is important to make is that while outwardly a sufferer and and their family may appear calm and collected, inside they are torn apart. They are scared, depressed, angry, and confused, but they fight hard not to ever show it. I was amazed at how Chris held herself together at all of Abby's graduation parties in May only to get home and breakdown. We all need to know that when others are going through this, what we see is far from the reality.
Family is critical. Both Chris' and my family have been fantastic. They have cared for our kids (with Chris' sister Debbie giving up her entire summer without hesitation), driven up numerous times from Pennsylvania (her brother Tim and sister Sally) and called almost daily (see comments below on blogs). Her parents have been fantastic. My family has also been great, always asking what they can do to help, sending love, being there when we need them.
It takes a village. I have written about this before, but more than anything this was the single largest lesson learned for Chris and I. We have been blown away at how our extended community has reached out to help us. This village, made of neighbors, life long friends, family, church members, colleagues at work, and even unknown people, have reached out to help and offer support. I cannot say enough times how valuable the meals, the rides to the doctors, the phone calls, the cards, the prayers, the small gifts offering hope have been. A great best friend coordinated all meals for many many weeks, to the point we had to say thanks but no more. Another has called up after dinner and said, "you did not walk today, lets go now", even though I know she was tired. Another drove her to Boston for entire day medical appointments on their only day off. Friends from her high school in Belgium have called and left many messages of support. Friends of our parents from all over the US have sent cards. Friends at IBM from Singapore, Sydney, Paris, all over, have sent their well wishes ( including a colleague in NJ who herself has been very sick and sent a great note of inspiration). Friends from UNH, Univ. of Delaware, a student doing a semester in New Zealand. On Chris' 100th day, we got cards from people we do not know, including a great card from a gentleman in Philadelphia who gave Chris some words of encouragement. It all has been absolutely beyond anything I had ever thought possible. For Chris, she has been so pleased to hear from friends, it means alot that people call to check on her. At this point, Chris now feels very good when she can give back, or "pass it forward". She did the breast cancer walk, she has been helping others in need, and she is really looking forward to getting back involved in much of the charity work she did prior to getting sick. It takes a village to take care of a very sick person, and this village of ours ( a worldwide village) has been the single most amazing thing for us in helping.
Communications. This is a hard one as it is complex. When we first entered this surreal world, we had no idea what to share, what to hold back, how to tell people, how to talk to our kids. Based on what I now know, the best approach is always one of complete and open communication. Tell anyone who wants to know the whole story, the good and the bad. There is no sense in hiding the reality. Some people will be very interested, others have their own issues and will listen and wish you good luck. One of the toughest decisions we had to deal with is what we would say to our children. We let them ask the questions but also tried to explain it all. We did lessen the degree of risk of the transplant/chemo. For someone with severe cardiac involvement like Chris, the chance of death during the first 100 days was about 20%. We knew this very well, but we probably hid that reality more than anything else. Maybe this was selfish on our part, but we did not want to deal with the emotional panic of our children while we needed to be focused on Chris. We wanted them to live as normal of a summer as possible, so we tried to give them only the positive. In retrospect, that was the right decision. The other lesson is the power of the blog. It has been invaluable. It has helped me give updates to hundreds at a time, it has been therapeutic for me, in fact very therapeutic, and it has let me share this ordeal with others who are or will go through it. One thing that was very hard for me was to answer the phone all evening long when Chris was unable to talk, giving an update on how she was. We would have very long days at the Center, I would make Chris a dinner and then clean both the dinner dishes as well as the food when it came back up, and then the phone would ring. I was exhausted and just wanted to rest and focus in getting her comfortable. Yet the calls were mostly from our families and I knew they were calling with their love. The blog has allowed me to give updates and people can read them at their convenience. One decision I made that I strongly feel is the right one was not to open it up for comments. This would have put pressure on me to respond, and more importantly I felt people would feel obligated to say something every time. We knew just by reading it that people cared, but by not allowing comments, I believe it was easier for both sides.
I have been told by many people that they really appreciated the blog and found it very helpful. I am not a natural writer and have never done any writing like this, but I have found that the best way of communicating my thoughts was to write from the heart. This was the therapeutic side of it for me. Probably the biggest mistake I have made is getting too focused on the medical elements - the details of the blood tests, the description of the disease, the medications, etc. Chris has read very little of this, literally a paragraph or two on a given day. When this is all over, I will somehow package these posts all together, from the beginning, and let her read them. She remembers very little, but I think she will find it very interesting. I occasionally have gone back and looked at random days. It has been an incedible ride and I am glad I have documented it. My hope is that as new patients enter into this craziness, they can at least see the details of one story. Chris and I were incredibly lucky that we had Jen and Steve Gershman to help guide us through, but there is very little documented, maybe this will help some. WHEN we are successful, then those scared to death like we were can maybe see actual hope.
Friends. Never ever try to watch the entire 10 year series of Freinds. Trust me on this one. There is clear evidence of acute brain damage to those who try. Yet as I write that, it has been our Friends who have done so much for us. Friends have been the single most important element of Chris' success and yet here I am warning people to avoid watching Friends. Not being a writer, I don't know if that is a juxtaposition, a contradiction, or the antithesis of each other, but it is at least interesting to me.
I think that at this point I have more than tried the patience of the readers on my "Lessons Learned". I apologize, but wanted to get it documented. I know I have editorialized, complained, over-described, and bored some to death with this blog, but I really appreciate your reading it. We are not done by any means with Chris' journey to health. We see Dr. Falk in 3 weeks,, we go back for a three day evaluation at BU in March, and Chris continues to work to get her body back to normal. We are trying to live a normal life now, and feel pretty optimistic. We went out for dinner last night with friends and ran into many other couples from around town. To me, it was almost like the old days (i.e. Jan. '08). We spoke about our kids, the town, real estate, jobs, etc, and little about Chris' illness. She has been through absolute hell and and here we are, less than a year from diagnosis, and trying to get back to a normal life. I look at her when she is talking to others and I feel so much pride and amazement.
OK, sorry for the far too long note. More in a few weeks, thanks for checking, please remember to look again down the road. It means so much to Chris when people call and say hello. Please feel free to call, send a note, give a prayer, or just wish her well.
-If your family member, colleuege, neighbor, whomever says, "I'm just not feeling right" or "something is wrong but I can't tell you what" and this goes on for an extended period (more than a few weeks), get it checked out. Don't write it off to old age or work stress or a low-grade fever. I am convinced the body sends the mind clear messages that attention is needed. If something isn't feeling right, then do somehting about it. We all want to fight the battle, keep moving, go to work, etc. We don't have time for the Doctor. Lesson: If you don't feel well for more than a few weeks, see a doctor. Time may be very important. Many Amyloid patients miss their opportunity for treatment because they were not diagnosed early enough. They die from a lack of a diagnosis.
-Get a second opinion on anything more than the basics. As I have stated many times, medicine is an art not a science. What one doctor misses, the other may see. Every doctor has a different set of experiences and training. They use their judgement based on what they know. The experts based at the BU center believe that >95% of primary care physicians have never diagnosed nor treated Amyloidosis and would not even think of testing for it. Maybe they read about it in Medical School. This is why the majority of sufferers die from the disease before treatment. Doctors don't see it, they don't know what too look for, and they don't even think to test for it. A great book to read if your looking for something on this topic is a book I happened to have read about a year ago. It is very interesting reading for a caregiver or advocate:
http://www.amazon.com/How-Doctors-Think-Jerome-Groopman/dp/0618610030 (sorry I don't mean to promote Amazon). I strongly recommend it before a crisis hits and I am sure it shaped my own thinking as Chris' advocate.
Have an annual physical with complete blood and urine tests. The body is filled with bio-markers which are indicators of chemical balance. I had no idea how complicated the chemical make-up of the human body is until I looked at a 5 page blood analysis. We have every metric on Chris since May and each one tells a story: glucose, potassium, protein, lambda light chains, albumin, creatinine, etc, etc...... Always have complete blood work and a urinalysis at every checkup. and always have it if you are going in if you don't feel well. Be aggressive about getting these done, they are not needless tests, they are critical chemical indicators. Chris had a urine test, which then led to a 24 hour urine analysis, which then led to an indication of an immuniglobulin M-spike, which then led to a bone marrow biopsy, and then a fat-pad biopsy that was tested with the famous red congo stain confirming Primary Amyloidosis. Without the first urine test, the whole sequence would have been delayed and the diagnosis may never have happened.
Become an expert. Whether it is heart disease, lung cancer, pneumonia, or any strange disease nobody has ever heard of, the resources are there to become an expert. The more you know, the more you become a participant in the discussion with the medical team vs an observer to the process. You can challenge, ask intelligent questions, seek out specialists, manage the drugs, demand tests, and potentially avoid problems. I now know drug interactions, I know all clinical trials by drug companies, I know the latest testing techniques, and I have read almost every paper written in the last few years on the subject. I use Google Alerts to scan the Internet for all mention of Amyloidosis as well as any publications from selected experts in the field. I get a weekly update on all new items about the disease, including new trials, published studies, conferences, etc. I suggest reading all recently published works. In our case it comes form magazines such as Blood, Journal of the British Hematological Society, etc.
Document and get a copy of everything. I have a copy of every single test result Chris has had. I have a copy of every report written by every doctor. I have the daily blood tests results as well as the graphs of the trends over the entire period. These are documents that are your right to have as they are about you or the patient you are advocating for. I used to think there was some special underground/behind the scenes data that only the medical experts had access to. In fact you have rights to everything. There are many benefits to this:
-You can become smarter by looking up every term used, understanding every test result, and getting a very well documented position of the doctors opinion.
-You can make these available to other doctors who need to know the background, especially those providing a second opinion.
-You might be able to avoid tests. Chris has had many many lung x-rays. I am concerned about over use of these. With a copy of the x-rays, I simply hand them to another doctor and avoid the tests. As I have learned, hospitals operate as members of competitive organizations. They often network well inside of their partnership, but not well outside to other partnerships.
Hospitals are very infectious places. One surprising lesson I have learned is how hospitals are really filled with germs. Chris' immunity system was completely wiped out, and they did not want to have her stay in the hospital for fear of infection. Some hospitals do the stem cell transplant and high-dose chemo as in-patient. Boston Medical insists that all patients live off-site, but close. The doctors strongly believe that they have a lower mortality rate simply due to the number one cause of death for these patients - infections. I am not advocating that patients avoid the hospital, but I was surprised at how many stories I heard about people getting very serious infections in the hospital such as MRSA, staff infections, etc.
There are two critical roles: Caregiver and Advocate. These can be the same person or two different people, but they both need to be in place. The caregiver is focused on the patient and his/her comfort. All seriously ill patients need a caregiver, even if at the hospital. Nurses have many patients to worry about cannot give the level of comfort or attention that an ill patient really needs. The caregiver needs to do a virtual brain transplant and think in the mind of the patient. What would make them more comfortable, who might they be worrying about, what are they feeling? The caregiver needs to swallow their pride completely. As Steve G, husband of Jen (the couple whom we read about in the paper back in May) told me," be prepared to wear a loincloth, you will become a slave and will need to swallow all pride and be a servant". This is a tough and frustrating job. You may be asked to get something very small from a sound sleep, you may have to clean up some really nasty stuff, you may be sent to the store to get something only to find it was the wrong thing. My suggestion is to just acknowledge that you are there to serve. It is not about you, it is totally, 100% about the patient. You get very little sympathy, very little acknowledgement, and few people understand what you are personally going through. Suck it up, be tough, and focus only on the patient. You will have to run on the internal pride you will develop that you are making a difference.
The other key role is the medical advocate. This is the person who needs to be the brains to the caregivers heart. Write everything down, understand all medications, understand the rationale behind all tests. If there is a need for medical attention, go get it. Get the best you can, even if you have to fight a battle. Question everything -not to dispute it, but to understand it. Bring a notebook to all medical appointments and listen in on all medical rounds if in the hospital. Listen very carefully and then question for clarity. Since medicine is an art, not a science, there is no simple algorithm that doctors use to come up with the answer. The advocate needs to be a part of the decision making process if the patient cannot be. Don't let things happen around you with others making the decision, be a part of the decision. Be aggressive, actively representing the patient. This does not mean being a pain in the ass. I have asked the doctors at BU if they thought I was overly aggressive and a negative in the process. The answer is always: "active participation is always better than benign neglect". Yes, I asked alot of questions and yes I knew what I was talking about (sometimes not as much as I thought I did), but they respected me for being involved. I witnessed some spouses who did not go into an appointment with the doctor, could not even properly say the disease, had no idea what was going on, and thus could not advocate. The advocate is not about making the patient comfortable (that is the caregiver), but it is about fighting the required battles in the complex medical system we live in. It is very hard to do both, but it can be done. Just think of them as two different roles and understand which one your in. The caregiver has no pride and a big heart, the advocate has a big brain and a strong enough ego to go into battle if required. (As I right this, I know it sounds so obvious to most of us, but I witnessed such distant participation and bad care giving by family members that it shocked me).
Hospital chairs are terrible beds. It is a very small price to pay from what Chris has been through, and as the caregiver in the hospital, Chris wanted me there at night. But, these chairs are torture devices. The interesting thing is the difference in the patients. I had a very big back operation a year ago and was in the hospital for a week. The absolute last thing I would want is for Chris to be there overnight. In fact her being there for more than an hour was tough. When I am sick, just leave me alone, don't ask me how I am doing, just let me be and I will let you know when I am better and I'll call you to come pick me up. Chris is the opposite. She wanted me there every night and all day. I had to just accept it (the caregiver has no rights to personal comfort as the lowest form of life on earth) and sleep in a chair. Forget the previously cured back, but that is another story. The nurses were always very good about finding me a blanket and pillows and sneaking me a muffin or a soda, but all I can suggest is try to avoid these chairs as best you can. Again, a very small price to pay and probably my only complaint worth sharing.
Rely on religion, meditation, poems, psychologists, or denial - whatever works. The human mind is sometimes the patients worst enemy. Chris and I spent many many nights up all night, scared to death of our future, what would happen to our fantastic life, will we ever get through this, etc. Many tears, night sweats, all night pacing, it was horrendous. We both needed help, some kind of guidance. Chris reached out to many alternatives: our minister, prayer books, meditation, Reiki, massage, acupuncture, lucky bracelets from the kids, etc. Each worked a little and helped in the total picture. One thing that I found interesting was when we met with the Psychiatrist at BU as part of the normal regiment. He told us a very effective coping mechanism was the use of denial as a way to deal with this. Deny that anything could go wrong, deny that this is really happening, deny that there will be any changes in your life. He told us that this is how many patients cope. To me, it is a dangerous approach, but probably very effective. Chris found her prayer book very useful as she went to bed. It focused on hope, life, and love. She also got a bracelet from a good friend that said: Expect Miracles, Have Faith. She wears it daily and really believes that with faith, miracles can happen. One point I think is important to make is that while outwardly a sufferer and and their family may appear calm and collected, inside they are torn apart. They are scared, depressed, angry, and confused, but they fight hard not to ever show it. I was amazed at how Chris held herself together at all of Abby's graduation parties in May only to get home and breakdown. We all need to know that when others are going through this, what we see is far from the reality.
Family is critical. Both Chris' and my family have been fantastic. They have cared for our kids (with Chris' sister Debbie giving up her entire summer without hesitation), driven up numerous times from Pennsylvania (her brother Tim and sister Sally) and called almost daily (see comments below on blogs). Her parents have been fantastic. My family has also been great, always asking what they can do to help, sending love, being there when we need them.
It takes a village. I have written about this before, but more than anything this was the single largest lesson learned for Chris and I. We have been blown away at how our extended community has reached out to help us. This village, made of neighbors, life long friends, family, church members, colleagues at work, and even unknown people, have reached out to help and offer support. I cannot say enough times how valuable the meals, the rides to the doctors, the phone calls, the cards, the prayers, the small gifts offering hope have been. A great best friend coordinated all meals for many many weeks, to the point we had to say thanks but no more. Another has called up after dinner and said, "you did not walk today, lets go now", even though I know she was tired. Another drove her to Boston for entire day medical appointments on their only day off. Friends from her high school in Belgium have called and left many messages of support. Friends of our parents from all over the US have sent cards. Friends at IBM from Singapore, Sydney, Paris, all over, have sent their well wishes ( including a colleague in NJ who herself has been very sick and sent a great note of inspiration). Friends from UNH, Univ. of Delaware, a student doing a semester in New Zealand. On Chris' 100th day, we got cards from people we do not know, including a great card from a gentleman in Philadelphia who gave Chris some words of encouragement. It all has been absolutely beyond anything I had ever thought possible. For Chris, she has been so pleased to hear from friends, it means alot that people call to check on her. At this point, Chris now feels very good when she can give back, or "pass it forward". She did the breast cancer walk, she has been helping others in need, and she is really looking forward to getting back involved in much of the charity work she did prior to getting sick. It takes a village to take care of a very sick person, and this village of ours ( a worldwide village) has been the single most amazing thing for us in helping.
Communications. This is a hard one as it is complex. When we first entered this surreal world, we had no idea what to share, what to hold back, how to tell people, how to talk to our kids. Based on what I now know, the best approach is always one of complete and open communication. Tell anyone who wants to know the whole story, the good and the bad. There is no sense in hiding the reality. Some people will be very interested, others have their own issues and will listen and wish you good luck. One of the toughest decisions we had to deal with is what we would say to our children. We let them ask the questions but also tried to explain it all. We did lessen the degree of risk of the transplant/chemo. For someone with severe cardiac involvement like Chris, the chance of death during the first 100 days was about 20%. We knew this very well, but we probably hid that reality more than anything else. Maybe this was selfish on our part, but we did not want to deal with the emotional panic of our children while we needed to be focused on Chris. We wanted them to live as normal of a summer as possible, so we tried to give them only the positive. In retrospect, that was the right decision. The other lesson is the power of the blog. It has been invaluable. It has helped me give updates to hundreds at a time, it has been therapeutic for me, in fact very therapeutic, and it has let me share this ordeal with others who are or will go through it. One thing that was very hard for me was to answer the phone all evening long when Chris was unable to talk, giving an update on how she was. We would have very long days at the Center, I would make Chris a dinner and then clean both the dinner dishes as well as the food when it came back up, and then the phone would ring. I was exhausted and just wanted to rest and focus in getting her comfortable. Yet the calls were mostly from our families and I knew they were calling with their love. The blog has allowed me to give updates and people can read them at their convenience. One decision I made that I strongly feel is the right one was not to open it up for comments. This would have put pressure on me to respond, and more importantly I felt people would feel obligated to say something every time. We knew just by reading it that people cared, but by not allowing comments, I believe it was easier for both sides.
I have been told by many people that they really appreciated the blog and found it very helpful. I am not a natural writer and have never done any writing like this, but I have found that the best way of communicating my thoughts was to write from the heart. This was the therapeutic side of it for me. Probably the biggest mistake I have made is getting too focused on the medical elements - the details of the blood tests, the description of the disease, the medications, etc. Chris has read very little of this, literally a paragraph or two on a given day. When this is all over, I will somehow package these posts all together, from the beginning, and let her read them. She remembers very little, but I think she will find it very interesting. I occasionally have gone back and looked at random days. It has been an incedible ride and I am glad I have documented it. My hope is that as new patients enter into this craziness, they can at least see the details of one story. Chris and I were incredibly lucky that we had Jen and Steve Gershman to help guide us through, but there is very little documented, maybe this will help some. WHEN we are successful, then those scared to death like we were can maybe see actual hope.
Friends. Never ever try to watch the entire 10 year series of Freinds. Trust me on this one. There is clear evidence of acute brain damage to those who try. Yet as I write that, it has been our Friends who have done so much for us. Friends have been the single most important element of Chris' success and yet here I am warning people to avoid watching Friends. Not being a writer, I don't know if that is a juxtaposition, a contradiction, or the antithesis of each other, but it is at least interesting to me.
I think that at this point I have more than tried the patience of the readers on my "Lessons Learned". I apologize, but wanted to get it documented. I know I have editorialized, complained, over-described, and bored some to death with this blog, but I really appreciate your reading it. We are not done by any means with Chris' journey to health. We see Dr. Falk in 3 weeks,, we go back for a three day evaluation at BU in March, and Chris continues to work to get her body back to normal. We are trying to live a normal life now, and feel pretty optimistic. We went out for dinner last night with friends and ran into many other couples from around town. To me, it was almost like the old days (i.e. Jan. '08). We spoke about our kids, the town, real estate, jobs, etc, and little about Chris' illness. She has been through absolute hell and and here we are, less than a year from diagnosis, and trying to get back to a normal life. I look at her when she is talking to others and I feel so much pride and amazement.
OK, sorry for the far too long note. More in a few weeks, thanks for checking, please remember to look again down the road. It means so much to Chris when people call and say hello. Please feel free to call, send a note, give a prayer, or just wish her well.
Wednesday, December 31, 2008
Way overdue update- The Holidays and Cardiologist
My apologies upfront for those checking the blog, your interest and support are great and I feel terrible that I have not kept things as updated as intended. There has been a lot going on and I will try to provide the latest.
Christmas was hard on Chris. Not physically, but emotionally. She loves the holiday and to her it represents the best family time of the year. So while she was thrilled to have everyone home, she was worried how many more of these she would have. She was switching between the joy of having everyone around with the fear of the future. It was the most negative and depressed I had seen her in months. We had my entire family as well as her parents over for Christmas Eve (23 people) and she worked her tail off to make it happen. It was fantastic and she pulled it all off. I played a surprise Santa for the neighbors next door (they did not even know it was me for a long time) and we all had a good laugh. Yet when it came time to go the midnight service at Church, she was too exhausted to go. She loves this candlelight service and it really puts the holiday into perspective for us all. But we went without her on her urging and returned home to her being very upset and depressed. It was the lowest I had seen her since July. I know that holidays can be extremely tough on people, and Chris wanted hers to be perfect. Yet I completely miscalculated how difficult it was on her emotionally. She was so tired, and had such conflicting emotions around the family all being there while being so scared of the future. It was a tough night for her and I blame myself for not preventing this. A lesson learned.
Christmas morning was fun and Chris did well. We opened stockings and presents and had a good breakfast with a very beautiful white snow outside. She seemed to have lost her sadness and was glad that her parents spent the night. We then went to my sisters for dinner. It was a blast (she knows how to hold a party!). The dinner was great, my Aunt joined us as well (so now 24 people) and the food was fantastic. Chris enjoyed it and really had a great time. Yet, she did not join the "dance party" where the adults and the teenagers went into a big time party mode. We had the music cranked and the place was jumping. What a blast. Chris never has been much of a dancer, but it would have been nice to see her rocking out. So Christmas Day was a very good one after a tough Christmas Eve.
The following Saturday (the 27th) was Chris' birthday. We all were up at her parents in NH and all of her siblings (Tim, Sally, and Debbie) made it up from NJ and PA to help her celebrate along with all but one niece/nephew (who was in Denver). She had a good time, a good dinner, and received some nice gifts. Again, I think this may have been a bit tough emotionally as well, as these milestones often cause one to think about the future.
Today, 12/31, we had the long awaited meeting with Dr. Falk - the cardiologist in Boston. Despite 8 inches of snow here, we made it in. Chris did the stress test that she did poorly on a month earlier. This one went much better. We then met with him and discussed the results - briefly. To make it simple, and to reconfirm my now strengthening hypothesis - Medicine is an art, not a science. We took Dr Falk through the BU results from early December and basically he dismissed them saying it was not possible to see such a reduction in the Ejection Fraction. The BU cardiologist had it at 25%, and today we heard "not possible". In fact, he was very upbeat, saying that based on her stress test results and his clinical observation, she was doing very well. He gave her the green light to start yoga, continue daily moderate exercise, and potentially start an even more aggressive exercise routine. We clearly have conflicting results from two different doctors. This is very frustrating, and of course we believe the more positive results. He wants us to have BU send the actual CD (not just the report) to him so he can see them directly. As I have stated earlier, I am not sure how doctors in different organizations work together, but when I see them dismiss anothers perspective, it is very disconcerting. We have to make our own decisions as to whom we believe and who's direction we follow. Clearly an art, not a science.
We will have the actual data sent from BU to Dr Falk and we will meet with him in 3 weeks - Jan 22nd to be exact.
So we walked out of the office today feeling very positive. We asked about the potential for a second stem cell transplant/high dose chemo OR the oral chemo. He said he would wait for the March 3 day analysis to give us his perspective.
So to wrap up the year, it has been a hell of a ride. Chris started what we thought would be a normal year last January, in April we heard the word Amyloidosis for the first time, in May she was confirmed with it, in June she had all her stem cells in her body removed and was given an almost lethal dose of poison (chemo), and in July she returned home 30 pounds lighter, no hair, no immune system, no strength, and in a distant stupor. She sat listless, never smiled, never did anything on her own, and watched life go by. Yet, she has worked relentlessly to get herself back to a normal life. She walks daily, is very independent, and actually yells at me like the good old days. I can't believe I am saying this, but it is so great to here her say "Steve, stop that" or "slow down" or "fix this". Of course she usually says it nicely, but I will take it any way she gives it. Chris has also seen both friends and fellow sufferers pass away from this terrible disease. It scares the daylights out of us, and in fact sets us way back emotionally after we work so hard to rebuild our confidence and optimism.
But now, on the last day of December of 2008, we end the year very optimistic. Chris told the doctor today feels better now than she did a year ago. That is progress, that is medicine, that is the power of prayer, that is the result of hundreds of well wishers all genuinely caring about Chris. She has reconnected with old friends, she has experienced more love than she ever thought possible, she has leaned on many people and they have supported her and she has verified that her family and friends are the most valuable people in the world.
For me, I have learned more than I thought possible. I have learned about blood disease, about medicine, about hospital practices, about how doctors think, about clinical trials, support groups, drug research, mortality rates, bio-markers, and how the human body rejects the poison of chemo by attempting to force it flying out of all ends of the body. And I have learned how to clean that up after that as well. But more important than the medical side of things, I have learned an amazing amount about the human side of this. I have seen what complete fear of death looks like, I have seen how a community has given all they possibly can to help a friend in need, I have seen a sibling give up months with her own family to take care of ours, I have seen my colleagues at IBM offer their help and support, and I have seen a very brave and strong woman fight a killer disease like a prizefighter. She may get knocked down, but she gets right back up again and goes the next round. She is amazing.
I have owed my Top 10 lessons learned for months now. I think I first promised back in July. My hope is to write those this coming weekend. I pray nobody ever has to go through what we have been through, but there has been a great deal of learning and I owe it to everyone to share.
I wish you all a very Happy New Year. Drink a toast to both Chris and yourselves as you usher in the new year. I will drink a toast to all of you!!!
And again, my apologies for my delayed posts. I know how many people check it regularly.
Christmas was hard on Chris. Not physically, but emotionally. She loves the holiday and to her it represents the best family time of the year. So while she was thrilled to have everyone home, she was worried how many more of these she would have. She was switching between the joy of having everyone around with the fear of the future. It was the most negative and depressed I had seen her in months. We had my entire family as well as her parents over for Christmas Eve (23 people) and she worked her tail off to make it happen. It was fantastic and she pulled it all off. I played a surprise Santa for the neighbors next door (they did not even know it was me for a long time) and we all had a good laugh. Yet when it came time to go the midnight service at Church, she was too exhausted to go. She loves this candlelight service and it really puts the holiday into perspective for us all. But we went without her on her urging and returned home to her being very upset and depressed. It was the lowest I had seen her since July. I know that holidays can be extremely tough on people, and Chris wanted hers to be perfect. Yet I completely miscalculated how difficult it was on her emotionally. She was so tired, and had such conflicting emotions around the family all being there while being so scared of the future. It was a tough night for her and I blame myself for not preventing this. A lesson learned.
Christmas morning was fun and Chris did well. We opened stockings and presents and had a good breakfast with a very beautiful white snow outside. She seemed to have lost her sadness and was glad that her parents spent the night. We then went to my sisters for dinner. It was a blast (she knows how to hold a party!). The dinner was great, my Aunt joined us as well (so now 24 people) and the food was fantastic. Chris enjoyed it and really had a great time. Yet, she did not join the "dance party" where the adults and the teenagers went into a big time party mode. We had the music cranked and the place was jumping. What a blast. Chris never has been much of a dancer, but it would have been nice to see her rocking out. So Christmas Day was a very good one after a tough Christmas Eve.
The following Saturday (the 27th) was Chris' birthday. We all were up at her parents in NH and all of her siblings (Tim, Sally, and Debbie) made it up from NJ and PA to help her celebrate along with all but one niece/nephew (who was in Denver). She had a good time, a good dinner, and received some nice gifts. Again, I think this may have been a bit tough emotionally as well, as these milestones often cause one to think about the future.
Today, 12/31, we had the long awaited meeting with Dr. Falk - the cardiologist in Boston. Despite 8 inches of snow here, we made it in. Chris did the stress test that she did poorly on a month earlier. This one went much better. We then met with him and discussed the results - briefly. To make it simple, and to reconfirm my now strengthening hypothesis - Medicine is an art, not a science. We took Dr Falk through the BU results from early December and basically he dismissed them saying it was not possible to see such a reduction in the Ejection Fraction. The BU cardiologist had it at 25%, and today we heard "not possible". In fact, he was very upbeat, saying that based on her stress test results and his clinical observation, she was doing very well. He gave her the green light to start yoga, continue daily moderate exercise, and potentially start an even more aggressive exercise routine. We clearly have conflicting results from two different doctors. This is very frustrating, and of course we believe the more positive results. He wants us to have BU send the actual CD (not just the report) to him so he can see them directly. As I have stated earlier, I am not sure how doctors in different organizations work together, but when I see them dismiss anothers perspective, it is very disconcerting. We have to make our own decisions as to whom we believe and who's direction we follow. Clearly an art, not a science.
We will have the actual data sent from BU to Dr Falk and we will meet with him in 3 weeks - Jan 22nd to be exact.
So we walked out of the office today feeling very positive. We asked about the potential for a second stem cell transplant/high dose chemo OR the oral chemo. He said he would wait for the March 3 day analysis to give us his perspective.
So to wrap up the year, it has been a hell of a ride. Chris started what we thought would be a normal year last January, in April we heard the word Amyloidosis for the first time, in May she was confirmed with it, in June she had all her stem cells in her body removed and was given an almost lethal dose of poison (chemo), and in July she returned home 30 pounds lighter, no hair, no immune system, no strength, and in a distant stupor. She sat listless, never smiled, never did anything on her own, and watched life go by. Yet, she has worked relentlessly to get herself back to a normal life. She walks daily, is very independent, and actually yells at me like the good old days. I can't believe I am saying this, but it is so great to here her say "Steve, stop that" or "slow down" or "fix this". Of course she usually says it nicely, but I will take it any way she gives it. Chris has also seen both friends and fellow sufferers pass away from this terrible disease. It scares the daylights out of us, and in fact sets us way back emotionally after we work so hard to rebuild our confidence and optimism.
But now, on the last day of December of 2008, we end the year very optimistic. Chris told the doctor today feels better now than she did a year ago. That is progress, that is medicine, that is the power of prayer, that is the result of hundreds of well wishers all genuinely caring about Chris. She has reconnected with old friends, she has experienced more love than she ever thought possible, she has leaned on many people and they have supported her and she has verified that her family and friends are the most valuable people in the world.
For me, I have learned more than I thought possible. I have learned about blood disease, about medicine, about hospital practices, about how doctors think, about clinical trials, support groups, drug research, mortality rates, bio-markers, and how the human body rejects the poison of chemo by attempting to force it flying out of all ends of the body. And I have learned how to clean that up after that as well. But more important than the medical side of things, I have learned an amazing amount about the human side of this. I have seen what complete fear of death looks like, I have seen how a community has given all they possibly can to help a friend in need, I have seen a sibling give up months with her own family to take care of ours, I have seen my colleagues at IBM offer their help and support, and I have seen a very brave and strong woman fight a killer disease like a prizefighter. She may get knocked down, but she gets right back up again and goes the next round. She is amazing.
I have owed my Top 10 lessons learned for months now. I think I first promised back in July. My hope is to write those this coming weekend. I pray nobody ever has to go through what we have been through, but there has been a great deal of learning and I owe it to everyone to share.
I wish you all a very Happy New Year. Drink a toast to both Chris and yourselves as you usher in the new year. I will drink a toast to all of you!!!
And again, my apologies for my delayed posts. I know how many people check it regularly.
Sunday, December 21, 2008
Very Tough Week - Physically and Emotionally
The week before Christmas has been a pretty difficult one for Chris unfortunately. She has had two bumps in the road - yet remains stalwart. Actually to call them bumps in the road minmmizes them - let's call them detours.
Wednesday was my third day down in NY attending some very tough meetings. I had flown down early Monday for 4 days of meetings while Chris and Stephen remained home. All was going very well so Stephen left Wednesday afternoon to go to Maine skiing with friends. At about 10:30 PM while I was dragging myself to bed after a very long day, my phone rang. It was Chris. She was breaking out in hives with rash across her body, her lips swelling, incredible itching, etc. This came on relatively suddenly. She called a friend who had been giving her some shots - the blood thinner coumadin. As a nurse, her friend has been very helpful as Chris hates needles (imagine the hundreds and hundreds of injections she has had this year). Her friend suggested she take some benadryl and call the doctor. Of course we had none in the house ( bad luck on our side ) so a scramble of calls started in the neighborhood and some was found (good luck except for those getting phone calls late at night). Her doctor called her back and said, "get to the ER - STAT". So without hesitation, our great friend Sally said "grab a coat, lets go". No kids were home, I was not home, and here is Chris heading to the ER at 11:00 at night. I won't bore you with the details, but Chris has had a very severe reaction to ==> we have no idea! 3 days letter, she is still breaking out with a very ugly rash across her torso, on her neck, under her arms. Big, red, raised welts. The ER treated the symptoms (prednisone, more benadryl), but did not identify the root cause.
This could have been caused by the coumadine, it may have been due to a new pill (same prescription, just different manufacturer) she started to take, possibly a couple of injections she needed prior to the coumadin, or even that Pad Thai she had for lunch. She got back to the house just before 3:00 AM and Sally spent the night in case of any further problems. Here is Sally getting into her own bed and 5 hours later she is getting back from the ER to sleep in another house. She was amazing - as she always is. I was pretty much useless other than irritating phone calls to Chris as she spoke to the ER physician. For so many months I have been her caregiver and medical advocate and here I was 200 miles away in NY - not a position I like being in.
So she is still suffering from the rash. She woke up Saturday morning with it all over her, wanting to itch everywhere, literally jumping up and down wanting to get out of her own skin. Large doses of benadryl and the prednisone help, but if we don't stay on top of it, she breaks out really badly. This all of course has just added to her frustration. As we drove to Burlington VT to pick up Melissa at the end of her semester, her frustration really showed. She is "so sick of being sick". "Why is this happening to me?", etc. I know well when she is on the verge of wanting to just breakdown and let it all out, but she allows herself to complain, maybe a tear or two, and she pulls herself together. She is a rock.
We will continue to look for the cause of the reaction. We have been in contact with her primary doctor, her cardiologist, and Boston center and they are working together to determine the next steps. In the meantime she is not taking any coumadin (or pad thai for that matter).
So Saturday, Chris and I drove to Burlington in the snow to move Melissa out of her house (in preparation to a semester in Australia starting next month). It was a very long day with about 6 hours of driving in the snow, packing her up, etc. We got home later than expected, yet ran to a party we had RSVP'd to earlier. We got there late and stayed relatively late. Upon our return home, she checked her mail before going to bed. This is the emotional detour, or crash I could say. As I have mentioned in earlier posts, Chris has been reading other peoples blogs who suffer from this terrible disease (yet still does not want to read this one). She reads the updates, prays for them, we talk about the differences with her care and their unique situations they all are going through. With me, she calls them by their first name, although she has never met them. "Paul had a good day today, Kevin is getting his heart transplant". The one blog she has been following since early fall has been a man in NY (Paul) with 2 young kids who went through the stem cell transplant and high dose chemo a few weeks after her. His wife and caregiver has been faithfully documenting his journey and Chris has felt very attached to the story (and Paul). He went home, she was thrilled, he had dialysis and she felt bad for him. Chris read yesterdays update and it threw her and I an unexpected shot to the head - Paul died of cardiac failure that morning. Two boys, 3 years old and 9 months old, a young wife who had been his caregiver, advocate, emotional support, etc. are left behind. They fought this battle as Chris has, with fortitude, optimism, many many tough periods, and with an incredible determination to beat this and get back to a normal life. Chris is devastated. Such a long, difficult, yet courageous battle only to have lost it in the end. Chris is scared, angry, confused, and very very sad for the family. This has thrown me for a loop as well, a big loop, as it brings the reality home. I can't share my emotions with Chris when she needs strength to lean on, but damn. DAMN THIS THING!
If you want to read a very tough story, here is Pauls blog:
http://gettingpaulhealthy.blogspot.com/2008/12/very-sad-day-indeed.html
Chris and I will get our act together and face the holidays with the joy of the season. We will have my entire family together and see almost all of hers in the next week or so. She has had a hell of a week, but she will do great. Keep praying for her. I'll give another update before Christmas.
Wednesday was my third day down in NY attending some very tough meetings. I had flown down early Monday for 4 days of meetings while Chris and Stephen remained home. All was going very well so Stephen left Wednesday afternoon to go to Maine skiing with friends. At about 10:30 PM while I was dragging myself to bed after a very long day, my phone rang. It was Chris. She was breaking out in hives with rash across her body, her lips swelling, incredible itching, etc. This came on relatively suddenly. She called a friend who had been giving her some shots - the blood thinner coumadin. As a nurse, her friend has been very helpful as Chris hates needles (imagine the hundreds and hundreds of injections she has had this year). Her friend suggested she take some benadryl and call the doctor. Of course we had none in the house ( bad luck on our side ) so a scramble of calls started in the neighborhood and some was found (good luck except for those getting phone calls late at night). Her doctor called her back and said, "get to the ER - STAT". So without hesitation, our great friend Sally said "grab a coat, lets go". No kids were home, I was not home, and here is Chris heading to the ER at 11:00 at night. I won't bore you with the details, but Chris has had a very severe reaction to ==> we have no idea! 3 days letter, she is still breaking out with a very ugly rash across her torso, on her neck, under her arms. Big, red, raised welts. The ER treated the symptoms (prednisone, more benadryl), but did not identify the root cause.
This could have been caused by the coumadine, it may have been due to a new pill (same prescription, just different manufacturer) she started to take, possibly a couple of injections she needed prior to the coumadin, or even that Pad Thai she had for lunch. She got back to the house just before 3:00 AM and Sally spent the night in case of any further problems. Here is Sally getting into her own bed and 5 hours later she is getting back from the ER to sleep in another house. She was amazing - as she always is. I was pretty much useless other than irritating phone calls to Chris as she spoke to the ER physician. For so many months I have been her caregiver and medical advocate and here I was 200 miles away in NY - not a position I like being in.
So she is still suffering from the rash. She woke up Saturday morning with it all over her, wanting to itch everywhere, literally jumping up and down wanting to get out of her own skin. Large doses of benadryl and the prednisone help, but if we don't stay on top of it, she breaks out really badly. This all of course has just added to her frustration. As we drove to Burlington VT to pick up Melissa at the end of her semester, her frustration really showed. She is "so sick of being sick". "Why is this happening to me?", etc. I know well when she is on the verge of wanting to just breakdown and let it all out, but she allows herself to complain, maybe a tear or two, and she pulls herself together. She is a rock.
We will continue to look for the cause of the reaction. We have been in contact with her primary doctor, her cardiologist, and Boston center and they are working together to determine the next steps. In the meantime she is not taking any coumadin (or pad thai for that matter).
So Saturday, Chris and I drove to Burlington in the snow to move Melissa out of her house (in preparation to a semester in Australia starting next month). It was a very long day with about 6 hours of driving in the snow, packing her up, etc. We got home later than expected, yet ran to a party we had RSVP'd to earlier. We got there late and stayed relatively late. Upon our return home, she checked her mail before going to bed. This is the emotional detour, or crash I could say. As I have mentioned in earlier posts, Chris has been reading other peoples blogs who suffer from this terrible disease (yet still does not want to read this one). She reads the updates, prays for them, we talk about the differences with her care and their unique situations they all are going through. With me, she calls them by their first name, although she has never met them. "Paul had a good day today, Kevin is getting his heart transplant". The one blog she has been following since early fall has been a man in NY (Paul) with 2 young kids who went through the stem cell transplant and high dose chemo a few weeks after her. His wife and caregiver has been faithfully documenting his journey and Chris has felt very attached to the story (and Paul). He went home, she was thrilled, he had dialysis and she felt bad for him. Chris read yesterdays update and it threw her and I an unexpected shot to the head - Paul died of cardiac failure that morning. Two boys, 3 years old and 9 months old, a young wife who had been his caregiver, advocate, emotional support, etc. are left behind. They fought this battle as Chris has, with fortitude, optimism, many many tough periods, and with an incredible determination to beat this and get back to a normal life. Chris is devastated. Such a long, difficult, yet courageous battle only to have lost it in the end. Chris is scared, angry, confused, and very very sad for the family. This has thrown me for a loop as well, a big loop, as it brings the reality home. I can't share my emotions with Chris when she needs strength to lean on, but damn. DAMN THIS THING!
If you want to read a very tough story, here is Pauls blog:
http://gettingpaulhealthy.blogspot.com/2008/12/very-sad-day-indeed.html
Chris and I will get our act together and face the holidays with the joy of the season. We will have my entire family together and see almost all of hers in the next week or so. She has had a hell of a week, but she will do great. Keep praying for her. I'll give another update before Christmas.
Saturday, December 13, 2008
Mixed News - as predicted
We heard from the doctors at Boston yesterday afternoon and it is not great news but more importantly it is not terrible news. In the end, it is progress, but will require us to continue the fight as it is not over. The results are what we actually had been predicting, as we are now smart enough to read the test results, ask the right questions, and know the options as the various meetings with doctors occur. I don't need to wait for a big report when I know the individual elements themselves. So, what I will describe is what we knew for the most part.
Lambda light chains: Normal is a number of 5-26. Chris it turns out was over 700 at one point and 660 when first diagnosed. She is now down to 39, and this represents a drop of 94% or so, but unfortunately still above 26. This means the amyloid proteins are still being produced, albeit at a significantly reduced rate. A 94% response is a long way there, but not across the finish line.
Plasma Cells in her bone marrow: Normal under 5%, Chris was over 10%. Now after the high dose chemo, she is back to under 5%. This is very good.
Serum IFE (immunoglubulin): This was down to zero, a very good story.
Flight Light Chain Ratio (Kappa/Lambda): Normal is .2-1.6. Chris is at .2, again very good.
So she still has the lambda free light chains being produced, but the biomarkers are all looking very good.
Cardio: Here is the difficult part, for both the doctors and for us. They cannot explain why the hematologic response has been so good while there continues to be further damage to her heart. We just got the analysis from the TEE (the echo through her esophagus) and it shows "severe left atrium enlargement", and "the right atrium is severely dilated". Further, there is "moderate to severe mitral regurgitation." They show an ejection fraction of 20%-25%, where normal is over 50%. Thus, as stated in earlier posts, our focus now shifts from the blood to the heart. We fully expect that there will be more work to do on the amyloidosis, as we need to stop the continued protein depostion, BUT, job #1 is now to understand and execute a plan that protects the heart. So the next activity is to meet with the Dr. Falk on December 31.
For those of you interested and looking for some technical and potentially mind-numbing/sleep inducing reading, here is a great paper written by Dr. Falk:
http://circ.ahajournals.org/cgi/reprint/112/13/2047.pdf .
I suggest only the very curious spend the time to print and read this, but it gives a detailed overview of the new battle front.
So enough of the technical stuff, lets talk about the most important element, Chris herself. Overall, she is doing very well emotionally and physically. She has been on the treadmill every day - this is her full time job, to ensure she is in top physical condition with the constraints she has. She has been very active, decorating the house, going to parties around town, shopping, etc. Outwardly, you would see little difference than the Chris you would have seen a year or two ago, except about 20 pounds lighter (she is up to a whopping 109) and very, very short hair (which is really starting to come back). She is upbeat, she is active, she is feeling good. However, there are times when we are both in the dump a bit. The worst time is late at night, when the mind has time to think a bit more. We both worry, about the future, about implications, about options, and about whether there is more we can be doing. I personally continue to ask myself; what else could we be doing? Are we missing a test? Are there better doctors to talk to? Am I prepared for all situations and outcomes? I hope so, but who knows for sure.
Overall, we are very fortunate. I can tell you when I first heard the word "amyloidosis" on Friday April 4th while touring Hartwick College with Abby, I had no idea what it is. Since then, Chris has had a stem cell transplant with high dose chemo, been "as close to hell as you can get and still being able to come back". returned home, and is living an active life. Melissa has written papers and made presentations on Amyloidosis at college, Abby has been an amazing help, cheerleader and supporter to Chris, and Stephen announced last week that for his required Senior Project at Worcester Academy, that he will be raising money for Amyloidosis research by riding from Florida to Holliston during his 2 week spring break - 1200 miles (more on that in future posts). So our family has been great. Yet, the most amazing thing has been what has occurred outside the family (which I know I state too often). Never ever, in my wildest dreams, did I ever expect a community to come together and help a friend like people have for Chris. It is the most amazing thing to see. Beyond anything I can describe. From the smallest things like a phone call to ask her how she is doing, to cards, to daily walks (sometimes in the rain and late at night in the neighborhood), the brownies, sauces, soups, meals, the errands, the interest, the listening, the learning, and most importantly the prayers and positive thoughts. It is beyond belief. There are no words strong enough or big enough to thank Chris' sister giving up her entire summer with her family to watch our family. I can't describe the incredible strength Chris has had in this fight, and I can't begin to express how optimistic I am for our future. We are going to fight two battles now (heart and blood), but I know the alignment of my tough wife, our amazing support (all of you), and the best medical care in the world will end up with success.
I'll try to update the blog occasionally over the next few weeks, and will provide a complete report after the meeting with Dr. Falk. Thanks for your continued interest.
Lambda light chains: Normal is a number of 5-26. Chris it turns out was over 700 at one point and 660 when first diagnosed. She is now down to 39, and this represents a drop of 94% or so, but unfortunately still above 26. This means the amyloid proteins are still being produced, albeit at a significantly reduced rate. A 94% response is a long way there, but not across the finish line.
Plasma Cells in her bone marrow: Normal under 5%, Chris was over 10%. Now after the high dose chemo, she is back to under 5%. This is very good.
Serum IFE (immunoglubulin): This was down to zero, a very good story.
Flight Light Chain Ratio (Kappa/Lambda): Normal is .2-1.6. Chris is at .2, again very good.
So she still has the lambda free light chains being produced, but the biomarkers are all looking very good.
Cardio: Here is the difficult part, for both the doctors and for us. They cannot explain why the hematologic response has been so good while there continues to be further damage to her heart. We just got the analysis from the TEE (the echo through her esophagus) and it shows "severe left atrium enlargement", and "the right atrium is severely dilated". Further, there is "moderate to severe mitral regurgitation." They show an ejection fraction of 20%-25%, where normal is over 50%. Thus, as stated in earlier posts, our focus now shifts from the blood to the heart. We fully expect that there will be more work to do on the amyloidosis, as we need to stop the continued protein depostion, BUT, job #1 is now to understand and execute a plan that protects the heart. So the next activity is to meet with the Dr. Falk on December 31.
For those of you interested and looking for some technical and potentially mind-numbing/sleep inducing reading, here is a great paper written by Dr. Falk:
http://circ.ahajournals.org/cgi/reprint/112/13/2047.pdf .
I suggest only the very curious spend the time to print and read this, but it gives a detailed overview of the new battle front.
So enough of the technical stuff, lets talk about the most important element, Chris herself. Overall, she is doing very well emotionally and physically. She has been on the treadmill every day - this is her full time job, to ensure she is in top physical condition with the constraints she has. She has been very active, decorating the house, going to parties around town, shopping, etc. Outwardly, you would see little difference than the Chris you would have seen a year or two ago, except about 20 pounds lighter (she is up to a whopping 109) and very, very short hair (which is really starting to come back). She is upbeat, she is active, she is feeling good. However, there are times when we are both in the dump a bit. The worst time is late at night, when the mind has time to think a bit more. We both worry, about the future, about implications, about options, and about whether there is more we can be doing. I personally continue to ask myself; what else could we be doing? Are we missing a test? Are there better doctors to talk to? Am I prepared for all situations and outcomes? I hope so, but who knows for sure.
Overall, we are very fortunate. I can tell you when I first heard the word "amyloidosis" on Friday April 4th while touring Hartwick College with Abby, I had no idea what it is. Since then, Chris has had a stem cell transplant with high dose chemo, been "as close to hell as you can get and still being able to come back". returned home, and is living an active life. Melissa has written papers and made presentations on Amyloidosis at college, Abby has been an amazing help, cheerleader and supporter to Chris, and Stephen announced last week that for his required Senior Project at Worcester Academy, that he will be raising money for Amyloidosis research by riding from Florida to Holliston during his 2 week spring break - 1200 miles (more on that in future posts). So our family has been great. Yet, the most amazing thing has been what has occurred outside the family (which I know I state too often). Never ever, in my wildest dreams, did I ever expect a community to come together and help a friend like people have for Chris. It is the most amazing thing to see. Beyond anything I can describe. From the smallest things like a phone call to ask her how she is doing, to cards, to daily walks (sometimes in the rain and late at night in the neighborhood), the brownies, sauces, soups, meals, the errands, the interest, the listening, the learning, and most importantly the prayers and positive thoughts. It is beyond belief. There are no words strong enough or big enough to thank Chris' sister giving up her entire summer with her family to watch our family. I can't describe the incredible strength Chris has had in this fight, and I can't begin to express how optimistic I am for our future. We are going to fight two battles now (heart and blood), but I know the alignment of my tough wife, our amazing support (all of you), and the best medical care in the world will end up with success.
I'll try to update the blog occasionally over the next few weeks, and will provide a complete report after the meeting with Dr. Falk. Thanks for your continued interest.
Thursday, December 11, 2008
Waiting for Godot (really Sanchorawala)
Chris has been very busy today and not had much time to be idle and thinking. That is a good thing. We are waiting for the big call from the medical center tomorrow afternoon where they will tell us what the indicators are for the degree of response. I know hundreds of people are waiting for the big HCR to be claimed, but based on some of the results, while I do not think we are there, I think we are close. The question I have been asked frequently, and a good one is: "At one point do they claim victory?" Is 95% close enough? Is 98%? The answer is pretty binary as I understand it. Your either have a complete response or you don't. If your body is still producing the amyloid proteins ( and as you know, this means the lambda free light chains), then we have to stop the production and the resulting deposition of them in the organs. More proteins mean more damage, and thus there is still work to be done.
My best guess is that they are going to say - "we are pleased, there is a good response, enjoy the holidays, come back in January and we'll retest and decide the action plan then".
As I thought a bit more last night about how to describe Chris' status, I would break it down into two areas: 1) Hematologically things are really looking good. 2) Cardiologically (a new word I just invented I think), things are OK but need a great deal of attention. I remain positive that if we can stop further heart damage, then Chris can move forward with a great and active (but not too active) lifestyle. Her positive attitude will make a huge difference going forward.
Chris did sleep very well last night. She has carried such a tremendous burden of stress that I know she felt as though she completed a major milestone yesterday. As she slept soundly this morning, I swear there was a smile on her face. This meant the world to me.
More tomorrow night or maybe early Saturday morning. I cannot say it enough - Thanks to all of you who care so much.
My best guess is that they are going to say - "we are pleased, there is a good response, enjoy the holidays, come back in January and we'll retest and decide the action plan then".
As I thought a bit more last night about how to describe Chris' status, I would break it down into two areas: 1) Hematologically things are really looking good. 2) Cardiologically (a new word I just invented I think), things are OK but need a great deal of attention. I remain positive that if we can stop further heart damage, then Chris can move forward with a great and active (but not too active) lifestyle. Her positive attitude will make a huge difference going forward.
Chris did sleep very well last night. She has carried such a tremendous burden of stress that I know she felt as though she completed a major milestone yesterday. As she slept soundly this morning, I swear there was a smile on her face. This meant the world to me.
More tomorrow night or maybe early Saturday morning. I cannot say it enough - Thanks to all of you who care so much.
Wednesday, December 10, 2008
Return Visit - Day 3
OK, a deep breath so I can think how to best make this understandable. Bottom line is two key messages: 1) all the test are not in yet, 2) the tests that are in show very mixed and confusing indications/results. Let me start with the bad and finish with the good.
Chris has a serious heart problem that has become worse since the spring. The number one issue, amongst many, is a significantly reduced ejection faction (EF). In simple terms, ejection faction is the % of blood pumped out of the heart with each heart beat. Normally this is in the range of 55% to 58%. In May, Chris' EF was 49%, not too bad. Today it is 35%. This has clearly worsened over the year. This is not due to the Chemo, but amyloid damage. This reduced EF is a symptom of the hardening of the left ventricle wall, which with reduced muscle elasticity has less ability to pump efficiently. There may also be some valve leakage between the atrium and the ventricle. What this all means is that Chris continues to have congestive heart failure. However, do not let the term 'failure' scare you as it did me. Failure in this case means that the heart is just not pumping at normal rates, so failure does not mean stoppage, it means reduction. The reduction in the pumping means that as her body calls for more oxygen as she exercises, climbs stairs, whatever, she will not be able to keep up with the demand. She would become easily fatigued, out of breath, and maybe have chest pounding. The cardiac story is not a good one, but she can function with normal activity and if the damage stops where it is, she can live a normal life while being careful. Nobody knows what further heart damage will occur going forward. I asked the question a hundred times, but nobody knows.
We see Dr. Falk (the most knowledgeable cardiologist in the world on this) again on December 31st. He now becomes an even bigger part of the game plan going forward since heart involvement becomes the single biggest issue we face.
OK, so now the better news. The other organs all are doing well, in fact her kidneys, which were problem number two after the heart, has actually improved since the chemo. There are a potpourri of blood and urine tests to measure kidney effectiveness. Almost all of these came back with improved results. Her kidneys are doing what they are supposed to be doing, they are seeing less amyloid proteins then they did before, and they are flushing them from the body better than before. One of the key tests is the amount of protein collected in a 24 hour urine sample (Chris hates carrying the jug around, but has now become a pro at it). Her Mg/24 hours were over 4000 in May, now they are about 2800, so this is a big drop and indicates a downward trend. But, to put it in perspective, normal is about 150 Mg/24 hours. As they explained it all today, the reduction will take as long as two years. I of course asked where we were on the reduction curve, ahead or behind what they would have expected for a good response and they said "6 months ahead of the curve". Obviously that is good.
The other key metric is the amount of lambda free light chains. Before, Chris was 660. Today she was 39. This is the single best news we have heard. This is a direct result of the chemo and indicates that the free light chain proteins that are created by her plasma cells and are floating around, combining and becoming insoluble in her organs have reduced considerably. This is about 94% reduction. Better than no reduction, better than 50% reduction, and better than 93% reduction. BUT, not a complete reduction. Normal is 15 -26. There are 4 elements that make up the criteria for a hematologic complete response (the famous HCR). Getting down to 26 or lower is one of them. The others are the Bone Marrow plasma cells at under 5% (she was at 10% in May), a Kappa/Lambda ratio between .26 and 1.65 and a good serum Immunofixation (IFE) test (too hard to explain here). The only test data we have at this point is the amount of lambda free light chains, and that is very good. The others we will get on Friday.
So now, the big question: Did we get a complete response? the answer is we do not yet know. We probably need to wait another month to see if the lambda's continue to reduce. To be honest, based on the discussions today, it is not clear if a complete response is possible. I seems to be unlikely at this point. The next big question is: what if it isn't complete response, now what?
Four options:
1) A second stem cell replant with high dose chemo (all over again), probably next spring/summer
2) An oral chemo, using a drug in trial called Revlimid
3) an oral chemo, using a drug in trial called Velcade
4) do nothing and watch.
Chris and I were very clear (more me than her) - we want to continue to be very aggressive. If they heard one word today it was "aggressive". Chris survived the pure hell of the high dose chemo this past year, and will do it again if its poison (and that is what it is) kills the rest of the bad plasma cells creating the proteins.
So here is the bottom line:
Chris has very bad heart damage, which we are seeking world class medical help to address. She will most likely be placed on an anticoagulant to prevent clots in her heart from causing a stroke.
The test results from this week are not all in, and thus we do not know what the prognosis is. The ones we do have are positive, but not where we need them to be. My guess is that they will ask her to come back in January and we will jointly decide the course of action.
So there is a lot we don't know.
Here is what I do know:
-Chris is tough as nails, an incredible fighter who is fighting the fight of her life
-We have found the best medical care possible - no second guessing on a single thing we have done
-We have the most amazing family, friends, colleagues (IBMers), and doctors we could have ever wished for
-The power of prayer, good wishes, concern, good meals, cards, phone calls, walks in the woods, etc have been the single most important factor in her success to date. All of you reading this blog are responsible for her progress to date. Thanks to everyone of you!!!
Chris has a serious heart problem that has become worse since the spring. The number one issue, amongst many, is a significantly reduced ejection faction (EF). In simple terms, ejection faction is the % of blood pumped out of the heart with each heart beat. Normally this is in the range of 55% to 58%. In May, Chris' EF was 49%, not too bad. Today it is 35%. This has clearly worsened over the year. This is not due to the Chemo, but amyloid damage. This reduced EF is a symptom of the hardening of the left ventricle wall, which with reduced muscle elasticity has less ability to pump efficiently. There may also be some valve leakage between the atrium and the ventricle. What this all means is that Chris continues to have congestive heart failure. However, do not let the term 'failure' scare you as it did me. Failure in this case means that the heart is just not pumping at normal rates, so failure does not mean stoppage, it means reduction. The reduction in the pumping means that as her body calls for more oxygen as she exercises, climbs stairs, whatever, she will not be able to keep up with the demand. She would become easily fatigued, out of breath, and maybe have chest pounding. The cardiac story is not a good one, but she can function with normal activity and if the damage stops where it is, she can live a normal life while being careful. Nobody knows what further heart damage will occur going forward. I asked the question a hundred times, but nobody knows.
We see Dr. Falk (the most knowledgeable cardiologist in the world on this) again on December 31st. He now becomes an even bigger part of the game plan going forward since heart involvement becomes the single biggest issue we face.
OK, so now the better news. The other organs all are doing well, in fact her kidneys, which were problem number two after the heart, has actually improved since the chemo. There are a potpourri of blood and urine tests to measure kidney effectiveness. Almost all of these came back with improved results. Her kidneys are doing what they are supposed to be doing, they are seeing less amyloid proteins then they did before, and they are flushing them from the body better than before. One of the key tests is the amount of protein collected in a 24 hour urine sample (Chris hates carrying the jug around, but has now become a pro at it). Her Mg/24 hours were over 4000 in May, now they are about 2800, so this is a big drop and indicates a downward trend. But, to put it in perspective, normal is about 150 Mg/24 hours. As they explained it all today, the reduction will take as long as two years. I of course asked where we were on the reduction curve, ahead or behind what they would have expected for a good response and they said "6 months ahead of the curve". Obviously that is good.
The other key metric is the amount of lambda free light chains. Before, Chris was 660. Today she was 39. This is the single best news we have heard. This is a direct result of the chemo and indicates that the free light chain proteins that are created by her plasma cells and are floating around, combining and becoming insoluble in her organs have reduced considerably. This is about 94% reduction. Better than no reduction, better than 50% reduction, and better than 93% reduction. BUT, not a complete reduction. Normal is 15 -26. There are 4 elements that make up the criteria for a hematologic complete response (the famous HCR). Getting down to 26 or lower is one of them. The others are the Bone Marrow plasma cells at under 5% (she was at 10% in May), a Kappa/Lambda ratio between .26 and 1.65 and a good serum Immunofixation (IFE) test (too hard to explain here). The only test data we have at this point is the amount of lambda free light chains, and that is very good. The others we will get on Friday.
So now, the big question: Did we get a complete response? the answer is we do not yet know. We probably need to wait another month to see if the lambda's continue to reduce. To be honest, based on the discussions today, it is not clear if a complete response is possible. I seems to be unlikely at this point. The next big question is: what if it isn't complete response, now what?
Four options:
1) A second stem cell replant with high dose chemo (all over again), probably next spring/summer
2) An oral chemo, using a drug in trial called Revlimid
3) an oral chemo, using a drug in trial called Velcade
4) do nothing and watch.
Chris and I were very clear (more me than her) - we want to continue to be very aggressive. If they heard one word today it was "aggressive". Chris survived the pure hell of the high dose chemo this past year, and will do it again if its poison (and that is what it is) kills the rest of the bad plasma cells creating the proteins.
So here is the bottom line:
Chris has very bad heart damage, which we are seeking world class medical help to address. She will most likely be placed on an anticoagulant to prevent clots in her heart from causing a stroke.
The test results from this week are not all in, and thus we do not know what the prognosis is. The ones we do have are positive, but not where we need them to be. My guess is that they will ask her to come back in January and we will jointly decide the course of action.
So there is a lot we don't know.
Here is what I do know:
-Chris is tough as nails, an incredible fighter who is fighting the fight of her life
-We have found the best medical care possible - no second guessing on a single thing we have done
-We have the most amazing family, friends, colleagues (IBMers), and doctors we could have ever wished for
-The power of prayer, good wishes, concern, good meals, cards, phone calls, walks in the woods, etc have been the single most important factor in her success to date. All of you reading this blog are responsible for her progress to date. Thanks to everyone of you!!!
Tuesday, December 9, 2008
Return Visit - Day 2
Not a great day today. I'll keep this short, as I really am not feeling like going into great detail and I am hoping that tomorrow will be better. Today was two sessions:
1) the support group. I have now been to five of these and each f them is different. Today there were a variety of experiences/stories. A woman from California was waiting on a heart and liver transplant, a man from NC had his transplant and high dose chemo 4 years ago and was doing great, another man had just localised impact in his stomach. Many different stories, but generally all good ones. So we walked out of that feeling good about these stories.
2) met with the Boston Medical cardiologist (not the one we saw two weeks ago). To be brutally honest, neither Chris or I like this guy, and we think it is more than just the message he gives. He has the sympathy of a rock and the heart of a piece of cold steel - just brutal. So here the news was not as positive as we were hoping for. There is continued decline in Chris' heart function, specifically her ejection fraction which is a measure of pumping effectiveness. There are some "biomarkers" or measurements of heart effectiveness that were not as good as they were previously. It was not a positive story and Chris and I walked out about as low as we have felt in the last 3-4 months. Tomorrow we will get the larger picture from the doctor we trust the most, but today was a huge stab in the back.
Despite the heart results, Chris continues to feel great. She honestly has a great attitude, has alot of energy, and is very positive. I think how she feels trumps what the chemical indicators show, but for me, it has been a very tough day. I'm hoping for a better day tomorrow.
1) the support group. I have now been to five of these and each f them is different. Today there were a variety of experiences/stories. A woman from California was waiting on a heart and liver transplant, a man from NC had his transplant and high dose chemo 4 years ago and was doing great, another man had just localised impact in his stomach. Many different stories, but generally all good ones. So we walked out of that feeling good about these stories.
2) met with the Boston Medical cardiologist (not the one we saw two weeks ago). To be brutally honest, neither Chris or I like this guy, and we think it is more than just the message he gives. He has the sympathy of a rock and the heart of a piece of cold steel - just brutal. So here the news was not as positive as we were hoping for. There is continued decline in Chris' heart function, specifically her ejection fraction which is a measure of pumping effectiveness. There are some "biomarkers" or measurements of heart effectiveness that were not as good as they were previously. It was not a positive story and Chris and I walked out about as low as we have felt in the last 3-4 months. Tomorrow we will get the larger picture from the doctor we trust the most, but today was a huge stab in the back.
Despite the heart results, Chris continues to feel great. She honestly has a great attitude, has alot of energy, and is very positive. I think how she feels trumps what the chemical indicators show, but for me, it has been a very tough day. I'm hoping for a better day tomorrow.
Monday, December 8, 2008
Return Visit - Day 1
Our first day back at the clinic in a long time, but it is very familiar to us and we are comfortable being there, strange as that sounds. We know may of the people, we know the building, we know the procedures, and we know all the terms. It is easy to feel like veterans having been through this previously. As before, and as we once were, there are people there that are going through this for the first time (the deer in the headlights look) and they have no idea what to expect. They have read that this is a fatal disease on the Internet and the average life expectancy. They don't know anything about the disease, the treatment, the doctors, they are just scared to death. Chris and I relate to this so well. We tried to start up conversations with the others going through their first three days and attempted to reassure them that they have found the best place to be. On the other side of the coin, we met a man today who had been diagnosed 4 years ago at the age of 70 and he also went through the stem cell transplant and high dose chemo and is doing well. So we are both givers and receivers of the all important "hope" that is the required ingredient for success.
Day 1 consisted of the following:
Blood Work and Vital Signs: Chris has many many vials of blood drawn today. They will analyze every possible aspect of this over the next 24 hours. Her blood pressure was a bit low (91/74) but not too bad. They will check her red blood cells, her white blood cells, and about 90 other unique tests. The lab results we received last time were 12 pages long.
Chest X-Ray: Chris has had many of these and to be honest I am getting a bit worried about all the radiation she must be getting. I would say she has had over a dozen x-rays in the last year on her chest/lungs. They are looking for pleural effusion - basically water in the lungs or surrounding chest cavity. This is an indication of congestive heart failure and was a problem she had pretty badly this spring. As with the blood test, we did not get any results.
Bone Marrow Biopsy: This is the dreaded big thick long needle inserted into the pelvis bone marrow. They remove a few large needles full. They are primarily looking at the % of plasma cells and the degree that their a light chain proteins in the plasma. Again, no results today.
Echocardiagram: This is the heart imaging procedure where the measure size, wall thickness, efficiency, etc. It is about a 40 minute test that they record to a DVD. Between the echo she had a few weeks ago, and the esophagus one done last Friday, they will have lots of data to look at.
Examination: This was the only meeting with a Doctor today. They asked her about a gazillion questions about her health, her medications, her activity, her emotions, and just about everything else. They were surprised to find out we went and saw the other cardiologist, but were interested in seeing his analysis. We had not met him before as he is a "fellow" new to the center, but he seemed like a good guy. I think I amazed him a bit with my knowledge of the disease, the tests, the "biomarkers", etc. I asked him questions about her BNP, her lambda numbers, her degree of left ventricle hypertrophy, etc. ( I have done a TON of research). He was a bit taken aback but acknowledged that much "homework" had been done. Nevertheless, we got no answers, only a "wait until Wednesday" response.
So the day was uneventful. We have no further insight, no good or bad results, just an ongoing level of nervousness about what we are going to hear later in the week.
I know many of you prayed a special prayer for Chris this week. It is not possible to tell you how much this means to us, but trust me, Chris feels the amount of love and good wishes being sent her way.
More tomorrow night after Day 2.
Day 1 consisted of the following:
Blood Work and Vital Signs: Chris has many many vials of blood drawn today. They will analyze every possible aspect of this over the next 24 hours. Her blood pressure was a bit low (91/74) but not too bad. They will check her red blood cells, her white blood cells, and about 90 other unique tests. The lab results we received last time were 12 pages long.
Chest X-Ray: Chris has had many of these and to be honest I am getting a bit worried about all the radiation she must be getting. I would say she has had over a dozen x-rays in the last year on her chest/lungs. They are looking for pleural effusion - basically water in the lungs or surrounding chest cavity. This is an indication of congestive heart failure and was a problem she had pretty badly this spring. As with the blood test, we did not get any results.
Bone Marrow Biopsy: This is the dreaded big thick long needle inserted into the pelvis bone marrow. They remove a few large needles full. They are primarily looking at the % of plasma cells and the degree that their a light chain proteins in the plasma. Again, no results today.
Echocardiagram: This is the heart imaging procedure where the measure size, wall thickness, efficiency, etc. It is about a 40 minute test that they record to a DVD. Between the echo she had a few weeks ago, and the esophagus one done last Friday, they will have lots of data to look at.
Examination: This was the only meeting with a Doctor today. They asked her about a gazillion questions about her health, her medications, her activity, her emotions, and just about everything else. They were surprised to find out we went and saw the other cardiologist, but were interested in seeing his analysis. We had not met him before as he is a "fellow" new to the center, but he seemed like a good guy. I think I amazed him a bit with my knowledge of the disease, the tests, the "biomarkers", etc. I asked him questions about her BNP, her lambda numbers, her degree of left ventricle hypertrophy, etc. ( I have done a TON of research). He was a bit taken aback but acknowledged that much "homework" had been done. Nevertheless, we got no answers, only a "wait until Wednesday" response.
So the day was uneventful. We have no further insight, no good or bad results, just an ongoing level of nervousness about what we are going to hear later in the week.
I know many of you prayed a special prayer for Chris this week. It is not possible to tell you how much this means to us, but trust me, Chris feels the amount of love and good wishes being sent her way.
More tomorrow night after Day 2.
Saturday, December 6, 2008
Heading into uncharted waters
This past week and this coming week are very strange for us. We really do not know what to expect, how to properly be prepared, and how to react to different scenario's. This past week has been a busy one for Chris on the medical front, but of course next week is the big one.
On this past Tuesday, Chris had a stress test in Boston with Dr. Falk, the cardiologist. The test was short as Chris has had a bad cold that she really has not been able to shake. Lot's of coughing, stuffiness, general malaise. She said she felt tired on the treadmill after 5 minutes, and her blood pressure dropped a bit, which concerned her. She generally walks about 45 minutes straight everyday, so it was a bit disconcerting to not do as well on the stress test as she would have expected. I think we all think(or hope) this was due to her cold. As such, she has been rescheduled for another stress test on December 31 - what a way to celebrate the end of a tough year.
After this appointment on Tuesday, she met with her primary care physician who put her on an antibiotic to try to get rid of this cold. That was Tuesday and having heard her cough most of the night last night, she has not seemed to have broken this yet. I am hoping today is a much better one for her.
Yesterday, she was at another Boston hospital having a transesophageal echocardiagram. They had to put her out for this as they put a device down her throat to look at her heart more directly. The whole intent here is to look at possible damage to the right atrium and determine whether there may be some kind of an exposure with the proteins that could possible cause a stroke. The treatment is to put her on a blood thinner, possibly for the rest of her life if stroke becomes a concern.
Chris' spirits have been a little lower in the past few days. I am not sure if this is due to her cold, her having to go back to the hospital for more prodding and probing this past week, or the uncertainty of this coming week. We both know that in less than a week our lives will be different than they are now. We have many questions, concerns, hopes, etc. If there is a 50% reduction in the free light chains ( a 50% hematological response) does that mean another high dose chemo next summer? )Below in the last paragraph of this post, I will explain "free light chains). What if it is 90% or 10%. Is there a direct relationship between the percent response and life expectancy? Have there been any new medicines or clinical trials we need to pursue and consider since this past summer? Do we take immediate action or wait for her to get stronger? Clearly a lot of questions running through our mind.
Many of our friends have called to provide words of encouragement in the last few days. Those are all well appreciated. I'll try to accelerate the pace of these posting over the next week as I know how much concern and genuine interest and support exists out there.
Free light chains: We all have a small number of the protein elements that are not attached to the normal plasma protein. Our bodies produce two types of these unattached protein molecules: kappa and lambda. We have small amount floating in our blood and there is a normal ratio between them. A normal range for us is between 3 and 19 mg/L of kappa light chains, 6 and 26 mg/L for lambda light chains, and a kappa/lambda ratio of 6 and 26. Chris' kappa light chains were normal, but her lambda light chains were 660 mg/L. Thus she had more than 33X the normal rate of these lambda light chains floating in her body. These are what end up connecting to each other and forming the insoluble proteins that get lodged in the organ. Our hope is that the chemo has taken these lambda light chains from 660 to under 26. That will be a Complete Hematologic Response (the famous HCR). In a nutshell, that is what we are looking for this coming week - elimination of the lambda free light chains in her body.
Sorry for the medical lesson, but I know many have asked for a little more detail.
Have a great weekend and watch for updates next week. Thanks for your prayers this weekend.
On this past Tuesday, Chris had a stress test in Boston with Dr. Falk, the cardiologist. The test was short as Chris has had a bad cold that she really has not been able to shake. Lot's of coughing, stuffiness, general malaise. She said she felt tired on the treadmill after 5 minutes, and her blood pressure dropped a bit, which concerned her. She generally walks about 45 minutes straight everyday, so it was a bit disconcerting to not do as well on the stress test as she would have expected. I think we all think(or hope) this was due to her cold. As such, she has been rescheduled for another stress test on December 31 - what a way to celebrate the end of a tough year.
After this appointment on Tuesday, she met with her primary care physician who put her on an antibiotic to try to get rid of this cold. That was Tuesday and having heard her cough most of the night last night, she has not seemed to have broken this yet. I am hoping today is a much better one for her.
Yesterday, she was at another Boston hospital having a transesophageal echocardiagram. They had to put her out for this as they put a device down her throat to look at her heart more directly. The whole intent here is to look at possible damage to the right atrium and determine whether there may be some kind of an exposure with the proteins that could possible cause a stroke. The treatment is to put her on a blood thinner, possibly for the rest of her life if stroke becomes a concern.
Chris' spirits have been a little lower in the past few days. I am not sure if this is due to her cold, her having to go back to the hospital for more prodding and probing this past week, or the uncertainty of this coming week. We both know that in less than a week our lives will be different than they are now. We have many questions, concerns, hopes, etc. If there is a 50% reduction in the free light chains ( a 50% hematological response) does that mean another high dose chemo next summer? )Below in the last paragraph of this post, I will explain "free light chains). What if it is 90% or 10%. Is there a direct relationship between the percent response and life expectancy? Have there been any new medicines or clinical trials we need to pursue and consider since this past summer? Do we take immediate action or wait for her to get stronger? Clearly a lot of questions running through our mind.
Many of our friends have called to provide words of encouragement in the last few days. Those are all well appreciated. I'll try to accelerate the pace of these posting over the next week as I know how much concern and genuine interest and support exists out there.
Free light chains: We all have a small number of the protein elements that are not attached to the normal plasma protein. Our bodies produce two types of these unattached protein molecules: kappa and lambda. We have small amount floating in our blood and there is a normal ratio between them. A normal range for us is between 3 and 19 mg/L of kappa light chains, 6 and 26 mg/L for lambda light chains, and a kappa/lambda ratio of 6 and 26. Chris' kappa light chains were normal, but her lambda light chains were 660 mg/L. Thus she had more than 33X the normal rate of these lambda light chains floating in her body. These are what end up connecting to each other and forming the insoluble proteins that get lodged in the organ. Our hope is that the chemo has taken these lambda light chains from 660 to under 26. That will be a Complete Hematologic Response (the famous HCR). In a nutshell, that is what we are looking for this coming week - elimination of the lambda free light chains in her body.
Sorry for the medical lesson, but I know many have asked for a little more detail.
Have a great weekend and watch for updates next week. Thanks for your prayers this weekend.
Friday, November 28, 2008
Giving Thanks
This Thanksgiving week has been an interesting, and good one. With all the kids home, Chris has been energized and she really has a very positive attitude and great spirits. She has enjoyed doing lots of activities with them (cooking, errands, visiting friends, etc.) and will clearly miss the girls when they leave at the end of the weekend. I have watched and am very pleased to see how them being around has made a difference in Chris' outlook. We had Thanksgiving dinner at my sister Judy's and Chris did great with a long day, no signs of tiring and a good appetite.
On Wednesday, Chris and I had an appointment with a cardiologist in Boston who is the world renowned expert on amyloid damage to the heart. He used to be part of the Boston Medical team but has since switched medical partnerships. Nevertheless he remains the "go to guy" on this subject. Again, yet another advantage of being in Boston where the world class health care and expertise just doesn't end. Dr. Falk has led the medical field in clinical analysis and we sought him out to get his perspective, validate what we were hearing at Boston Medical, and satisfy our own need to ensure we have engaged all possible expertise. I am not sure how the Boston Medical program will react to us seeking other opinions, but I am sure they will respect our need to leverage all options.
The appointment went well. Chris had an exam including an echocardiagram, had blood work done, and we spent a long time answering questions - providing descriptions of the history, the treatment, and the period back home. This has led to two next steps. On Tuesday, Chris will have a stress test on the treadmill as they measure blood pressure, heart activity, oxygen levels, etc. This will give us an indication of her level of fitness and her ability to increase her daily amount of exercise. If she shows that she can maintain her blood pressure (and not get light-headed) while she exerts herself, this will be a good sign. If on the other hand she gets winded easily, her chest hurts, and her BP drops, this will probably indicate the heart damage is more than maybe we had thought. Tuesday will be a big day.
On Friday, Chris is going to Brighams and Womens Hospital in Boston for the next procedure. Here, they will insert a camera down her throat and somehow (Chris and I have been trying to figure this out) will snake it to her right atrium in her heart where they will look at the heart wall. They are afraid of hardened proteins deposited in her heart wall and want to see to what extent they are there. These can actually break off as a clot and cause a stroke. To prevent that from happening they are considering placing her on a blood thinner such as coumadin.
So next week will be another important week for Chris' journey to health. This of course will be followed by the week we have been trying to patiently wait for. Chris and I are both clearly getting nervous as we get closer, knowing that what we hear in the next 2 weeks will impact us more than can be written. Good or Bad, our lives will be forever changed. I could write for hours as to what I mean by that, but suffice it to say we are hoping for the best, preparing for the worst.
No matter what happens (in my heart, I know a miracle is going to happen), Chris and I are both thankful for the incredible love, support, friendship, and compassion everyone has given. We had an amazing Thanksgiving as we are more thankful than we have ever been in our lives. We are thankful for family and friends, the fact that we have been able to find the best medical support in the world, the fact that we hopefully caught this early, and the fact that we have been able to be very aggressive in treating this disease. We all have much to be thankful for.
On Wednesday, Chris and I had an appointment with a cardiologist in Boston who is the world renowned expert on amyloid damage to the heart. He used to be part of the Boston Medical team but has since switched medical partnerships. Nevertheless he remains the "go to guy" on this subject. Again, yet another advantage of being in Boston where the world class health care and expertise just doesn't end. Dr. Falk has led the medical field in clinical analysis and we sought him out to get his perspective, validate what we were hearing at Boston Medical, and satisfy our own need to ensure we have engaged all possible expertise. I am not sure how the Boston Medical program will react to us seeking other opinions, but I am sure they will respect our need to leverage all options.
The appointment went well. Chris had an exam including an echocardiagram, had blood work done, and we spent a long time answering questions - providing descriptions of the history, the treatment, and the period back home. This has led to two next steps. On Tuesday, Chris will have a stress test on the treadmill as they measure blood pressure, heart activity, oxygen levels, etc. This will give us an indication of her level of fitness and her ability to increase her daily amount of exercise. If she shows that she can maintain her blood pressure (and not get light-headed) while she exerts herself, this will be a good sign. If on the other hand she gets winded easily, her chest hurts, and her BP drops, this will probably indicate the heart damage is more than maybe we had thought. Tuesday will be a big day.
On Friday, Chris is going to Brighams and Womens Hospital in Boston for the next procedure. Here, they will insert a camera down her throat and somehow (Chris and I have been trying to figure this out) will snake it to her right atrium in her heart where they will look at the heart wall. They are afraid of hardened proteins deposited in her heart wall and want to see to what extent they are there. These can actually break off as a clot and cause a stroke. To prevent that from happening they are considering placing her on a blood thinner such as coumadin.
So next week will be another important week for Chris' journey to health. This of course will be followed by the week we have been trying to patiently wait for. Chris and I are both clearly getting nervous as we get closer, knowing that what we hear in the next 2 weeks will impact us more than can be written. Good or Bad, our lives will be forever changed. I could write for hours as to what I mean by that, but suffice it to say we are hoping for the best, preparing for the worst.
No matter what happens (in my heart, I know a miracle is going to happen), Chris and I are both thankful for the incredible love, support, friendship, and compassion everyone has given. We had an amazing Thanksgiving as we are more thankful than we have ever been in our lives. We are thankful for family and friends, the fact that we have been able to find the best medical support in the world, the fact that we hopefully caught this early, and the fact that we have been able to be very aggressive in treating this disease. We all have much to be thankful for.
Subscribe to:
Posts (Atom)